Common difficulties
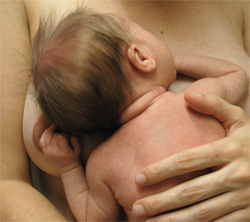
![]() At all times, skin-to-skin contact can help babies regain their natural sucking reflex. Strip your baby down to her diaper, remove your bra, and lay her skin-to-skin between your breasts. Place a blanket over her. Wait until she starts seeking out the breast, then gently guide her.
At all times, skin-to-skin contact can help babies regain their natural sucking reflex. Strip your baby down to her diaper, remove your bra, and lay her skin-to-skin between your breasts. Place a blanket over her. Wait until she starts seeking out the breast, then gently guide her.
![]() Remember, it’s normal for babies to cry (see Crying). It is also normal for your little one’s sleep pattern to be different from yours (see Sleep in the first weeks). This doesn’t mean that breastfeeding isn’t satisfying your baby.
Remember, it’s normal for babies to cry (see Crying). It is also normal for your little one’s sleep pattern to be different from yours (see Sleep in the first weeks). This doesn’t mean that breastfeeding isn’t satisfying your baby.
Moms who breastfeed may experience some difficulties, especially in the first few weeks. Fortunately, you can overcome several of them.
In the following pages, you’ll read about the most common difficulties and several suggestions for dealing with them. You can also refer to the table Breastfeeding difficulties for suggestions suitable to your situation. The key to overcoming most of the hurdles along the way is to go back to the basics (see Breastfeeding basics).
When to get help
It is better to consult a person trained in breastfeeding or a healthcare professional (see Getting help) if
- Your baby has difficulty latching on or is not actively sucking or regularly swallowing, even after you have followed the suggestions in this section
- You have nipple or breast pain or damage that doesn’t heal or get better even after you have followed the suggestions in this section
- Your baby pees less and has fewer bowel movements than is normal or isn’t putting on weight as expected for his age (see Is your baby drinking enough milk?)
- You’re worried about how much your baby is drinking or whether he is gaining weight
- You don’t notice a rapid increase in milk production between the 2th and the 5th day after your baby is born (see When your milk comes in)
If your baby still has dark, sticky stools (meconium) on the 5th day, see a health professional that same day.
You can call Info-Santé (8-1-1) at any time if you have any concerns.
Your baby has trouble latching on
Newborns don’t all develop at the same pace. Some take longer to learn how to latch on properly. If your baby cries and pushes on your breast, it’s because she’s hungry and can’t latch on. Don’t worry, she is not rejecting you.
Sometimes your baby won’t nurse because she can’t latch on. There can be a number of reasons for this, such as:
- You and your baby need to be better positioned (see Getting settled for a feed)
- You have
- firm, heavy, and tight (engorged) breasts
- flat or inverted nipples
- Your baby
- has difficulty sucking (e.g., a tight lingual frenum)
- has pain from the delivery (e.g., head, neck, collarbone)
- has had unpleasant experiences while breastfeeding (e.g., pressure on head, being forced to nurse)
In other cases, babies latch on but then let go. They don’t breastfeed long enough to get the milk they need. There are a number of reasons why your baby might have difficulty breastfeeding. For example
- She has jaundice that puts her to sleep
- She’s used to a bottle that flows faster
- You’re not producing enough milk, and she finds that the milk doesn’t flow fast enough
Most of the time, a combination of causes explains why your baby isn’t able to latch on.
What to do?
See the table Breastfeeding difficulties for suggestions specific to your situation.
Even if your baby can’t breastfeed right away, you can give her milk that you’ve expressed. During the first few days of learning to breastfeed, you can offer milk from a spoon or a little cup (see Offering milk from a spoon or cup). As the amount of milk she drinks increases, you can try giving a bottle (see Bottle-feeding your breastfed baby).
Counter pressure is another technique that can help your baby latch on if your breast is heavy, firm and tight (engorged) or if your nipple is flat or inverted (see Counter pressure).
Most babies will eventually learn to latch on, especially if you’re producing enough milk. Don’t hesitate to contact a trained breastfeeding support person for help (see Getting help).
Offering milk from a spoon or cup
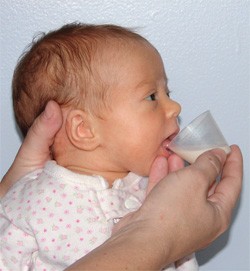
![]() If your baby isn’t getting enough milk from your breasts, you can use a cup.
If your baby isn’t getting enough milk from your breasts, you can use a cup.
Before you give your baby milk from a spoon or small cup, make sure she is awake and calm. Hold her on your lap and support her head. Bring the cup (or spoon) to her bottom lip and tilt it toward her tongue. Do not pour the milk in her mouth. The important thing is to follow your baby’s pace and appetite.
A trained breastfeeding support person can show you what to do and answer your questions.
Counter pressure
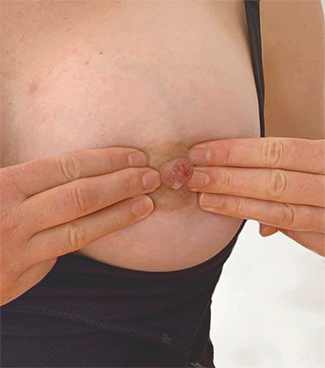
![]() Counter pressure involves pressing on the areola just before a feed.
Counter pressure involves pressing on the areola just before a feed.
Counter pressure can also help your baby latch on if your breast is firm, heavy and tight (engorged) or if your nipple is flat or inverted. Counter pressure involves gently pressing on the areola below the nipple just before feeding. Press with your fingertips for about one minute. Repeat by placing your fingers elsewhere on the areola to soften the whole area. You shouldn’t feel any pain.
Your baby used to nurse, but won’t anymore
Sometimes a baby who breastfed easily won’t nurse anymore. This can happen all of a sudden or come about gradually as he nurses less and less frequently.
If you know your baby is hungry, but he can’t seem to latch on or simply won’t take the breast, there are various possible explanations, such as:
- Your milk supply has decreased and your milk doesn’t flow fast enough for your baby.
- Your baby increasingly prefers the bottle, which flows faster.
- Your breasts are firm, heavy, and tight (engorged), and your baby has trouble latching on.
- You have an abundant supply of milk, and it flows very quickly.
- Your baby is sick or has a stuffy nose.
- Your baby is experiencing temporary discomfort (e.g., teething, stiff neck).
What to do?
See the table Breastfeeding difficulties for suggestions specific to your situation.
To compensate for the breastfeeding sessions he is skipping, you can continue to give him breast milk by expressing it. Try offering milk from a spoon or cup for the first few days (see Offering milk from a spoon or cup) or by bottle once he starts drinking larger quantities (see Bottle-feeding your breastfed baby).
If things aren’t back to normal after a few more attempts at breastfeeding, contact a trained breastfeeding support person (see Getting help).
Your baby only takes one breast
Some newborns feed more easily from one breast or seem to prefer one breast over the other. This is common, and quite often temporary
It’s possible that
- Your baby has some minor pain or discomfort related to the delivery (e.g., head, neck, collarbone) and might be less comfortable feeding on one side
- Your milk supply or milk flow is different in each breast
- Your nipples are different
What to do?
See the table Breastfeeding difficulties for suggestions specific to your situation.
It is preferable for your baby to take both breasts so she can drink as much milk as she needs. It’s therefore recommended that you
- Keep breastfeeding on the side where your baby is most comfortable
- Continue to offer the breast she seems to like least, without forcing her
- Express milk from the breast your baby takes less easily, to keep her fed and maintain your supply
Your baby sleeps a lot: should you wake him up for a feed?
Some babies sleep a lot and skip feedings, especially in the first 2–3 weeks. This makes it difficult for them to get all the milk they need.
If your baby sleeps a lot, you can let him sleep if he
- Wakes on his own to nurse 8 or more times every 24 hours
- Sucks actively and swallows regularly while at the breast
- Pees enough and passes enough stools per day (see Is your baby drinking enough milk?)
- Regains his birth weight within the first 2 weeks of life (see Weight gain)
If, on the contrary, your baby does not show these signs, wake him up to feed.
What to do?
If you have to wake your baby to nurse, start by placing him skin-to-skin with you.
Is he moving in his sleep, making sucking motions, or moving his eyes beneath his eyelids? These are signs that he is in a light sleep phase. Now is a good time to nurse him.
Your baby is not drinking enough milk during feedings
If your baby isn’t peeing enough or passing enough stools for her age, and especially if she isn’t gaining enough weight (see Is your baby drinking enough milk?), it might be a sign that she isn’t drinking enough breast milk. Consequently, she’s not getting enough nutrition.
There are a variety of possible reasons:
- She doesn’t nurse frequently enough or long enough.
- She sucks at the breast but doesn’t swallow enough milk.
What to do?
Make sure she nurses often enough, in other words at least 8 times every 24 hours, day and night.
You can express your milk so you can continue giving her breast milk. You can offer milk from a spoon or cup for the first few days (see Offering milk from a spoon or cup) or from a bottle once she starts drinking larger quantities (see Bottle-feeding your breastfed baby).
Contact a trained breastfeeding support person if things don’t quickly get better or if you have concerns (see Getting help).
You may need to supplement feedings with commercial infant formula to meet all your baby’s milk requirements.
To maintain breastfeeding despite the use of commercial infant formula, it is important to express milk to stimulate or increase your production. It’s a good idea to use a pump to express your milk every time you feed your baby with commercial infant formula.
Insufficient milk production
Many mothers think they don’t have enough milk, especially when their baby cries and wants to nurse often and for long periods. Remember, newborns cry for all kinds of reasons (see Crying). It is also normal for babies to nurse frequently (8 or more times per 24 hours) and even more frequently during a growth spurt (see Growth spurts).
Your breasts will become softer at the end of the day or after a few weeks of breastfeeding. This doesn’t mean you have less milk.
If your baby is peeing enough and passing enough stools and especially if he is gaining enough weight (see Is your baby drinking enough milk?), you can be sure that he is getting enough milk and that you are producing enough.
Sometimes, however, milk production is low right from the start of breastfeeding. In other cases, it can suddenly drop. This may or may not be temporary, and can be due to a number of different reasons:
- Your breasts are understimulated because:
- the number of feedings or expressing of milk is not enough in 24 hours (less than 8 times)
- there is a period of several hours (e.g., at night) when your breasts are not stimulated
- your baby’s suction is not strong enough
- the pump you’ve chosen doesn’t suit you or isn’t being used effectively
- your baby regularly takes a bottle
- your baby regularly drinks commercial infant formula
- You’ve had breast surgery (see If you’ve had breast surgery)
- You have a health problem (e.g., hormone disorder)
- You’re pregnant again (see If you’re breastfeeding—and pregnant)
- You’re taking oral contraceptives or a decongestant containing pseudoephedrin
Good to know...
Regardless of how much breast milk you produce, the quality of your milk is always excellent. Even in small amounts, breast milk provides your baby with a host of nutritional and immune elements that are not found in commercial infant formula.
What to do?
See the table Breastfeeding difficulties for suggestions specific to your situation.
Make sure your baby is well fed and continues to gain weight. Give him expressed milk or commercial infant formula. Even if you use infant formula, you can continue breastfeeding.
Generally speaking, the basic principle for maintaining or increasing your milk supply is to remove milk from the breasts at least 8 times every 24 hours, day and night. Some women need to get their milk out even more frequently. You can remove milk from your breasts by nursing your baby or expressing milk.
You can also talk to a trained breastfeeding support person who will help you assess your milk supply and determine how you can produce more, if you need to (see Getting help).
You have more milk than your baby needs (overproduction)
Once breastfeeding is established, some women produce more milk than their babies need. Even after feeding, their breasts are heavy and tight (engorged). There can be various reasons for an overproduction of milk. It may be related to factors such as
- The mother’s personal characteristics (e.g., having multiple children, being able to produce an abundance of milk)
- Regular expression of milk that the baby doesn’t need in addition to feedings
What to do?
Avoid expressing more milk than your baby needs.
Contact a trained breastfeeding support person (see Getting help). Overproduction can create difficulties.
Very fast milk flow (strong let-down reflex)
A few seconds after your baby starts nursing, you can hear her swallowing loudly. She may even choke a little, fuss or stop nursing and start crying as milk runs onto her face. Your baby is upset because the milk is flowing too quickly.
What to do?
If your milk starts flowing too fast, remove your baby from your breast for a few seconds and put her back on once the let-down reflex has passed.
Try different positions to see if there is one that suits you and your baby better. You can try laid-back position (see Getting settled for a feed). The milk will flow more slowly into your baby’s mouth in this position.
Breastfeeding difficulties
| You | What to do? |
|---|---|
| Are having difficulties finding the right position and bringing your baby to your breast | See Getting settled for a feed, and Bringing baby to your breast. |
| Have firm, heavy and tight (engorged) breas |
|
| Have flat or inverted nipples |
|
| Have insufficient milk supply |
|
| Your baby | What to do? |
|---|---|
| Has jaundice (see Newborn jaundice) |
|
| Has a tight lingual frenum that seems to be causing problems |
|
| Is experiencing pain or discomfort from the delivery (e.g., head, collarbone, tight neck muscles) |
|
| Has had unpleasant experiences at the breast |
|
| Nurses without swallowing |
|
| Has grown accustomed to bottle feeding |
|
| Cries while breastfeeding |
|
| Falls asleep or takes long breaks while breastfeeding |
|
| Is sick or has a stuffy nose |
|
| Is experiencing temporary discomfort (e.g., teething, stiff neck) |
|
Painful nipples
![]() Your nipples may be sensitive for the first few days, especially at the beginning of a feeding. Baby and mom are still in the learning period. After a few days, breastfeeding should not hurt.
Your nipples may be sensitive for the first few days, especially at the beginning of a feeding. Baby and mom are still in the learning period. After a few days, breastfeeding should not hurt.
![]() For many years, women with nipple pain were assumed to have thrush or a fungal infection. These days, nipple pain is usually associated with vasospasms (see Vasospasms) or muscle pain (see Muscle pain).
For many years, women with nipple pain were assumed to have thrush or a fungal infection. These days, nipple pain is usually associated with vasospasms (see Vasospasms) or muscle pain (see Muscle pain).
Are you feeling pain after the first 30 seconds of breastfeeding or are you afraid to nurse your baby because of the pain? The most common cause of pain is a poor latch. Improving how your baby latches on can significantly reduce nipple pain and damage (see Make sure your baby is latching on correctly).
Persistent pain or damage is one of the main reasons why women decide to stop nursing. Any pain or discomfort deserves attention. If you need to, contact a trained breastfeeding support person (see Getting help).
You have red or cracked nipples or a sore spot that sometimes bleeds
What it might be
Sore or cracked nipples
What to do?
- Vary breastfeeding positions (see Getting settled for a feed). If you need to reposition your baby, gently break the suction (see Breaking the suction).
- Try to improve how your baby latches on (see Bringing baby to your breast).
- Start nursing with the less sensitive breast.
- Take pain medication such as acetaminophen. A pharmacist can help you.
- If nursing is too painful, you can express your milk to feed your baby. Expressing milk also prevents engorged breasts and maintains your milk supply.
Consult a trained breastfeeding support person if the problem persists (see Getting help).
Over-the-counter ointments, balms, and creams won’t solve the problem, but may provide some relief.
You have an unpleasant sensation (e.g., burning, itching) and redness on your nipples
The sensation often persists between feedings and is more common in women who have eczema.
What it might be
A skin reaction to a new product or to moisture
What to do?
- Use washable nursing pads and avoid using disposable ones.
- Change the pads as soon as they are damp. Wash the pads in mild, unscented detergent.
- Stop applying creams, lotions, lanolin or other products on your nipples as you may be reacting to these products.
- Apply a thin layer of over-the-counter 0.5% hydrocortisone after every feeding for 3 to 5 days. There is no need to remove the product before you feed your baby. Ask your pharmacist for advice.
Consult a trained breastfeeding support person if the problem persists (see Getting help).
You have an unpleasant sensation (e.g., burning, pinching) in the nipple or throughout the breast, and your nipple changes colour (blue, white, or red)
This type of pain can occur after a feeding, between feedings, or upon contact with cold (e.g., getting out of the shower, grocery shopping in the frozen food aisle).
Nicotine, caffeine, and certain medications can aggravate the problem.
What it might be
A vasospasm
What to do?
- Check and correct the latch as needed (see Make sure your baby is latching on correctly).
- Keep your breasts and your body warm (e.g., dress warmly).
- Apply dry heat, such as the palm of your hand or a reusable heat pack, to the nipple immediately after feeding or when you see a change in colour.
Consult a trained breastfeeding support person if the problem persists (see Getting help).
You have a thin layer of skin or a small white dot on the nipple that blocks your milk
You may also have intense pain in the nipple and sometimes throughout your breast, especially at the beginning of a feeding.
What it might be
A blister
What to do?
- Avoid touching or scratching it (with your fingers or a needle).
- Continue to nurse. Your baby might pierce the blister as she feeds.
Consult a trained breastfeeding support person if you feel any pain or if the problem persists (see Getting help).
Painful breast
![]() For a long time, mothers were advised to “empty” their breasts when the breasts were engorged or in the presence of redness or a lump or hard area on the breast. We now know that it is better not to “empty” the breasts to avoid overproduction of milk.
For a long time, mothers were advised to “empty” their breasts when the breasts were engorged or in the presence of redness or a lump or hard area on the breast. We now know that it is better not to “empty” the breasts to avoid overproduction of milk.
Breast pain is often accompanied by redness or a lump or hard area on the breast. Any pain or discomfort warrants attention.
Some types of discomfort are associated with your milk coming in (see When your milk comes in) and with a normal level of engorgement during the first days or weeks of breastfeeding. Nursing effectively, frequently (8 or more times per 24 hours), and regularly (day and night) helps relieve discomfort, which typically lasts 24 to 48 hours.
Breast pain can affect breastfeeding and is one of the main reasons why women decide to wean their baby.
The following table shows the types of pain that lactating women may feel on one or both breasts, and some suggestions for relieving the pain.
You have tight, heavy breast
Can be painful
What it might be
Engorgement caused by excess milk or swelling
What to do?
Nurse your baby according to his needs.
- If your baby hasn’t drunk very much and you are uncomfortable, express a little milk after the feeding. Express just enough to be comfortable, without trying to empty your breasts.
- If your baby has difficulty latching on, express a little milk manually to soften the areola.
- Try to relax your breast by pressing on the areola near the nipple (see Counter pressure).
- Apply cold (e.g., ice or a cold washcloth) for 10 to 15 minutes every 1 to 2 hours between feedings to help reduce swelling and pain. Avoid heat.
- Massage your breasts lightly and gently (see How to do a “gentle massage”). Avoid deep massage, which can injure the breasts.
You have a bump or hard or red area on the breast
What it might be
Obstruction of one or more milk ducts caused by excess milk or swelling
What to do?
Nurse your baby according to his needs.
If you are uncomfortable after the feeding, express a little milk. Express just enough to be comfortable, without trying to empty your breasts.
- Apply cold (e.g., ice or a cold washcloth) for 10 to 15 minutes every 1 to 2 hours between feedings to help reduce swelling and pain. Avoid heat.
- Massage your breasts lightly and gently (see How to do a “gentle massage”). Avoid deep massage, which can injure the breasts.
- If needed, take ibuprofen (e.g., Advil®, Motrin®) to reduce redness, swelling, and pain.
- Acetaminophen (e.g., Tylenol®) may reduce pain.
Ask your pharmacist for advice.
You have a bump or a hard, swollen, or red area on the breast; fever and flu symptoms (e.g., aches, chills)
What it might be
Inflammation or infection (mastitis)
What to do?
- Nurse your baby according to his needs.
- Continue breastfeeding with the infected breast if you can; the milk is fine.
If your baby hasn’t drunk very much and you are uncomfortable, express a little milk. Express just enough to be comfortable, without trying to empty your breasts.
- Apply cold (e.g., ice or a cold washcloth) for 10 to 15 minutes every 1 to 2 hours between feedings to help reduce swelling and pain. Avoid heat.
- Massage your breasts lightly and gently (see How to do a “gentle massage”). Avoid deep massage, which can injure the breasts.
- Take ibuprofen (e.g., Advil®, Motrin®) as needed to reduce redness, swelling, pain and fever.
- Acetaminophen (e.g., Tylenol®) may also reduce pain and fever.
Ask your pharmacist for advice.
When to see a healthcare professional (see Getting help)
- Your symptoms have not started to improve after 24 hours.
- The situation is getting worse (e.g., the redness spreads, the skin texture changes, the hard area becomes very painful, fever lasts more than 24 hours or increases).
You may require antibiotics.
Muscle pain
You might experience pain in the breasts or nipples if you have or have had problems with your back, ribs, neck, or shoulders. Why? Because the nerves in those parts of the body are the same ones that govern sensations in the breasts and nipples.
What to do?
When you breastfeed, take the time to get comfortable. Support your back and keep your elbows close to your body. Your feet are flat on the floor or on a low stool.
You can also get settled in a laid-back or lying down position (see Getting settled for a feed).
Keep your spine and shoulders aligned at all times. Always try to sit on both buttocks.
Avoid
- leaning on the armrest and crossing your legs
- leaning forward by turning your body
- carrying your baby on one hip while moving around with him
If the pain persists, consult a muscle specialist (e.g., physiotherapist).
Areola: Darker area of the breast around the nipple.
Express: Pump or squeeze milk from the mother’s breast.
Mastitis: Inflammation of the breast. May also be an infection.
Overproduction of milk: Milk production that exceeds baby’s needs.


