The composition of human milk
Breast milk composition changes throughout the breastfeeding period to adapt to your baby’s needs and age.
Breast milk is made up of proteins, sugars, and all the fats your baby needs, including omega 3 fatty acids that support brain and eye development. It provides each baby with the exact amount of vitamins and minerals they need to develop, with the exception of vitamin D (see Vitamin D: Not your ordinary vitamin!). What’s more, it contains enzymes that facilitate digestion.
Breast milk has antibodies that help your baby fight infections and develop his immune system. It is also rich in good bacteria that are thought to provide him with lifelong protection.
To date, over 200 components have been identified in human milk. Certain factors influence the composition and taste of breast milk.
What influences the composition of milk
The mother’s diet
Drinking a lot of fluids doesn’t increase the amount of milk you produce. While you’re breastfeeding, you’ll naturally be thirstier than usual. Listen to your body—you don’t need to force yourself to drink a lot. However, if you notice your urine is dark or cloudy, it means you’re not drinking enough.
There aren’t any foods that increase milk production. Eat regularly and eat enough. You can also have snacks if you’re hungry.
Some foods can have a slight effect on the taste of the milk you produce, but your baby will adapt. Some studies suggest that it can help babies develop their taste for food if mothers eat a varied diet while breastfeeding.
Most breastfeeding mothers can eat whatever they like, including foods deemed risky during your pregnancy (i.e., sushi, deli meats, cheese).
If you think your baby is having a reaction to something you’re eating, read Breastfed babies and allergies.
![]() If you are a vegan (i.e., you don’t eat any animal products, that is, meat, fish, eggs or milk products) and you are breast-feeding, you should take a Vitamin B12 supplement.
If you are a vegan (i.e., you don’t eat any animal products, that is, meat, fish, eggs or milk products) and you are breast-feeding, you should take a Vitamin B12 supplement.
Eat foods rich in protein, iron, calcium and Vitamin D. It might be a good idea to consult a nutritionist.
Fish
Fish belongs on your menu. However, some fish species absorb pollutants that make their way into breast milk and could harm a baby. To take advantage of the benefits of eating fish while minimizing the risk from contaminants such as mercury, read Fish and Seefood.
Coffee, tea, chocolate, herbal tea and other drinks
Caffeine passes into breast milk. If you consume a lot of it, it can make your baby nervous and irritable until the caffeine is eliminated from his system. Caffeine is found in coffee, tea, energy drinks, chocolate, and some soft drinks.
Energy drinks are not recommended while breastfeeding because they contain other substances that might harm your baby.
Other products (coffee, tea, etc.), may be consumed in moderation, up to two cups or so per day.
Decaffeinated drinks such as cereal-based beverages and herbal tea can be good substitutes for caffeinated beverages.
Alcohol
Any alcohol consumed by a breastfeeding mother goes into her milk. It takes 2 to 3 hours to eliminate alcohol from breast milk, depending on the mother’s weight.
Alcohol can interfere with breastfeeding and may reduce milk production and lead to early cessation of breastfeeding.
Even though a breastfeeding baby only receives a tiny share of the alcohol his mother drinks, he eliminates it more slowly than an adult and his system is more sensitive to its effects. This can have harmful impacts, especially on the baby’s sleep habits.
Breastfeeding mothers can drink an occasional alcoholic beverage. The benefits of breastfeeding outweigh the risks of occasional light alcohol consumption.
If you do have a drink, you can reduce your baby’s exposure to alcohol in one of these ways:
- Breastfeed your baby right before having a drink.
- Or wait 2 to 3 hours per serving of alcohol before nursing again. After waiting, simply nurse normally at the next feeding.
If you have more than one serving, feed your baby milk you expressed in advance (frozen or refrigerated) while the alcohol remains in your system. You may need to express milk to relieve engorgement of your breasts, but this milk should be discarded because it contains more alcohol.
To find out how long it takes for your body to eliminate alcohol according to your weight, visit beststart.org/resources/alc_reduction/pdf/brstfd_alc_deskref_eng.pdf.
![]() Each serving or glass of an alcoholic beverage takes 2 to 3 hours to be eliminated from your blood and milk.
Each serving or glass of an alcoholic beverage takes 2 to 3 hours to be eliminated from your blood and milk.
If you have questions about alcohol consumption while breastfeeding, talk to your health professional or call the Motherisk Helpline at 1-877-327-4636.
Good to know
In Canada, one serving or 1 drink = 13.5 g (17 ml) of pure alcohol.
Size of a standard drink
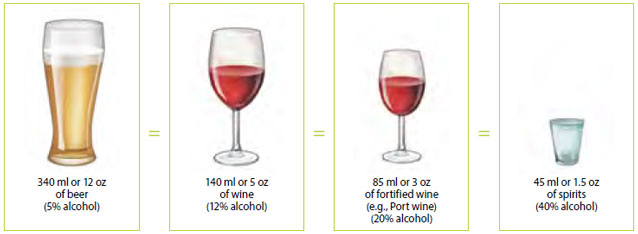
Illustrations: Maurice Gervais
Tobacco and electronic cigarette
![]() Use of tobacco, electronic cigarette, cannabis, or other drugs and exposure to second-hand smoke are not recommended while breastfeeding.
Use of tobacco, electronic cigarette, cannabis, or other drugs and exposure to second-hand smoke are not recommended while breastfeeding.
Tobacco can interfere with milk production. Nicotine from tobacco and electronic cigarette also passes through breast milk and can cause crying, irritability, and insomnia to the breastfed child. Try to avoid smoking or vaping just before feeding.
Talk to your doctor if you are thinking about using pharmacological aids such as patches or nicotine gum to quit smoking.
Even if you do smoke or vape, breastfeeding provides many benefits for you and your baby, including protecting him from respiratory infections.
Cannabis and other drugs
Cannabis and certain other drugs such as amphetamines, cocaine, heroin, LSD, and PCP pass into breast milk and are dangerous for your baby.
Cannabis use by a breastfeeding mother can result in irritability, shorter, less frequent feedings, and reduced muscle tone in the baby.
Medications
Most medications pass into breast milk, but in very small amounts. Some medications are a better choice because more is known about their effects on nursing babies.
Many medications may be taken while breastfeeding, including acetaminophen, ibuprofen and most antibiotics.
Decongestants containing pseudoephedrine can reduce milk production. It’s best to ask your pharmacist to recommend another product.
Talk to a health professional before taking any medication or natural health product. Some medications may decrease your milk supply or cause other problems.
It’s very rare to have to stop breastfeeding because of medical treatment. If a health professional advises you to stop breastfeeding because of a medication, here’s what you can do:
- Say that breastfeeding is important to you and your baby.
- Ask if there are any medications that can be taken while breastfeeding instead.
Exposure to contaminants
In Québec, environmental pollution is not generally a problem for breastfeeding mothers and babies.
Breastfeeding mothers who come in contact with or breathe in chemical substances contained in household products may pass these substances on in small amounts to their babies through breast milk. This is only a problem in the case of regular and prolonged exposure, such as occurs at work.
In day-to-day life, exposure to the following products on an occasional basis is nothing to worry about:
- At the hairdresser: hair styling products, dyes and perms
- At the dentist: local anaesthetic, fillings and root canals
- In the home: latex paint and varnish, home cleaning products
If you work in an environment where you are exposed to contaminants like solvents, inks or dyes that may be dangerous to your breastfed baby, you may be eligible for reassignment or preventative withdrawal. Visit cnesst.gouv.qc.ca/en/life-events/i-am-expecting-child for more information. You can also consult your doctor.
Antibodies: Substances made by the body to fight off disease. Also called immunoglobulins.
Express: Pump or squeeze milk from the mother’s breast.
Immune system: Organs and mechanisms that allow the body to fight against infections.


