When the unexpected happens
All parents want a healthy baby. But sometimes the happy event of childbirth can take an unpredictable turn.
Even under the best conditions, things may not go as planned. Having a family brings great joys, as well as its share of challenges and uncertainties.
If your baby suffers from an infection, birth defect, or other health problem she may require hospitalization after birth or in the days that follow. This comes as a shock to parents who must learn to live with this new reality and adjust to a role different from the one they imagined.
The birth may also occur before the date scheduled. Babies are considered premature when birth takes place before 37 weeks of pregnancy. A premature baby may require some of the special care presented below.
Care of premature babies
| Time of birth | Care |
|---|---|
| Before 34 weeks | Transfer to a neonatal intensive care ward in a hospital that has one. Your baby may
|
| 34 to 37 weeks | Extra care, but less of it. Your baby may
|
Some suggestions for getting through these difficult moments
You may feel guilty or helpless if your baby is hospitalized for a complication such as premature birth, infection, birth defect (whether discovered before or after birth) or another health problem. Here are a few suggestions to help you through these difficult times.
Ask questions
![]() Don’t hesitate to ask your child’s care team any questions you may have.
Don’t hesitate to ask your child’s care team any questions you may have.
Don’t be afraid to ask questions about your baby’s health and the care and treatment she’s receiving. If you have concerns about certain aspects or her care or treatment, ask if other options are available. She’s your baby and you are entitled to have a say in decisions affecting her.
It is the responsibility of members of the care team to keep you informed. However, time constraints sometimes make it hard to have these conversations. Ask them when is the best time to talk and find out when the doctor usually visits.
Ask for help and support
If possible, ask your family and loved ones to help you by taking care of the house or minding your other children. You may not always be able to be at the hospital, especially if you have other children.
In the case of a prolonged hospital stay, it’s essential that you get enough rest to stay healthy and to be able to care for your baby when she arrives or returns home. Remember that your child will need you not only during the hospitalization but afterwards as well.
Don’t hesitate to ask for psychological help if you feel you need it. Specialized care teams often include social workers and psychologists that can support you.
Find out about the resources available
The specialized care team at the hospital can advise about help you can receive at home. You can also request a follow-up with your CLSC when your child is discharged from the hospital. It’s important not to neglect the post‑hospitalization period, which may also be difficult for some parents.
If your baby has a particular health problem, check if there are resources for parents of children with the same problem. The help of other parents who face similar challenges can be useful.
The following website lists many resources available across Québec: laccompagnateur.org (in French only)
There is also an association to support parents of premature infants:
Préma-Québec
1-888-651-4909 / 450-651-4909
premaquebec.com
A few suggestions for making a hospital stay easier
Many parents want to be with their baby when she is hospitalized. Sometimes, the father and mother take turns staying with their baby during the day when they are able, or may want to spend the night. Check with your hospital about the options available.
For example, you can ask if the hospital has a room where you can room-in with your baby if you want to. Keep in mind, however, that some hospitals may have space constraints that make staying with your baby difficult.
Have physical contact with your baby in an incubator
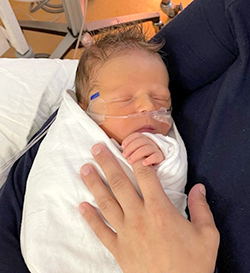
![]() Don’t hesitate to ask for help with touching your baby in the incubator or holding her in your arms or skin‑to‑skin under a blanket.
Don’t hesitate to ask for help with touching your baby in the incubator or holding her in your arms or skin‑to‑skin under a blanket.
Don’t hesitate to ask for help with touching your baby in the incubator or with holding her in your arms or skin‑to‑skin under a blanket. Your baby will feel your presence and this will help her. If you can’t take her out of the incubator, ask if you can put a scarf or piece of clothing that smells of you in beside her.
Breastfeed your hospitalized baby
Even if she is hospitalized, your baby may be able to nurse and take in part or all of the milk she needs. If you want to breastfeed, but your baby is not yet able to suck, it is important to stimulate your breasts in the hours after birth to get your milk production going (see Ways to make breastfeeding easier).
Express your milk until your baby can breastfeed on her own. Your milk can be refrigerated or frozen until she is ready for it. When you give her the milk, extra minerals or calories may be added to it if your baby needs them.
You can ask for help expressing your milk. Breast pumps are often available in intensive care wards. Don’t be discouraged if you get only a few drops the first few times. Your breasts need regular stimulation to produce what your baby needs.
Don’t forget that your baby has a tiny stomach and only needs a few drops of milk when first starting to breastfeed. Having a photo of your baby, being close to her, or making skin-to-skin contact for a few minutes beforehand can help you express more milk.
If you hadn’t planned to breastfeed, it’s not too late to think about it.
Ask about hospital visits
Some hospitals may allow visits by your other children or your loved ones. Make sure your visitors aren’t sick when they come to see your baby and that they don’t have any infections, such as a cold or a cold sore (oral herpes). Even an ordinary cold can be serious for your newborn.
It can be a good idea to talk with your other children about what’s going on. The baby’s siblings also have feelings and concerns about the baby’s health.
For example, you may wish to reassure them that what’s happening with the baby is not their fault. Slightly older siblings often believe that their feelings of jealousy toward the new baby have caused the complications. You can get them involved in caring for the newborn whenever possible.
Death of a newborn child
The loss of a baby is always an ordeal for the parents and family.
It is very rare for a baby to die before birth or in the first few days of life. The cause is usually extreme premature birth or birth defects.
When a baby dies during pregnancy, it is often recommended that the mother have a natural or induced vaginal delivery. After the delivery, it can be particularly difficult for her if she starts producing milk or has bloody discharge. These signs often act as reminders of the loss of the baby.
Grieving the loss of a baby
At the hospital some parents may ask to hold their baby in their arms, to dress her, or take photos. Doing so can help with the grieving process.
An autopsy may be performed to determine the cause of death. Various funeral options (e.g., cremation, burial) are usually suggested.
Back home it’s normal to experience feelings of shock, outrage, confusion, and sadness. The intensity and duration of these emotions will vary from person to person, as will and the amount of time needed to recover. The different phases of grief may overlap, and don’t always come in the same order. Also, the two parents often do not mourn in the same way or at the same pace.
Support resources

![]() Parents who have experienced the death of a newborn say that the support of their loved ones and groups for parents who have lost a child helped them through the ordeal.
Parents who have experienced the death of a newborn say that the support of their loved ones and groups for parents who have lost a child helped them through the ordeal.
Photo: Maude Lortie
Parents who have experienced the death of a newborn say that the presence and support of their loved ones helped them through the ordeal.
There are also support groups for parents who have lost a child. These groups can provide valuable assistance to parents as they go through the mourning period and allow them to share their experience with other bereaved parents.
Parents can also see a health professional (e.g., psychologist, social worker) for counselling, either individually or as a couple.
Consult your CLSC to find out about services offered there or other services in your area.
To find the CLSC in your area
Visit sante.gouv.qc.ca/en/repertoire-ressources/clsc.
Fondation Portraits d’Étincelles
Free photo and photo touch-up service for babies who died prior to or at birth (in French only)
1-877-346-9940
portraitsdetincelles.com
Parents Orphelins
Association québécoise des parents vivant un deuil périnatal
514-686-4880
parentsorphelins.org/en
Revenir les bras vides
CHU Sainte-Justine
A series of free videos and information documents on perinatal grief.
chusj.org/en/Care-Services/C/Pregnancy-Complications/Perinatal-bereavement
You can check with the Commission des normes, de l’équité, de la santé et de la sécurité du travail (CNESST) for details about absences and leave you may be entitled to.
Commission des normes, de l’équité, de la santé et de la sécurité du travail (CNESST)
1-844-838-0808
cnesst.gouv.qc.ca/en/working-conditions/leave/specific-situations/leave-event-termination-pregnancy
If your baby died after 19 weeks of pregnancy or after her birth, you may also be entitled to receive benefits under the Québec Parental Insurance Plan.
Québec Parental Insurance Plan
1-888-610-7727
rqap.gouv.qc.ca/en/wage-earner/death/death-of-a-child
Express: Pump or squeeze milk from the mother’s breast.
Birth defect: Abnormality existing at birth but that developped during pregnancy.


