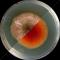
Epicoccum purpurascens
Basics
There are only two named species of Epicoccum, E. purpurascens (formerly known as E. nigrum) and E. andropogonis as well as many studied strains which are yet un-named {1794; 816; 3318}.
Taxonomy
| Kingdom | Fungi | Order | Pleosporales |
| Phylum | Ascomycota | Family | Leptosphaeriaceae |
| Class | Dothideomycetes | Genus | Epicoccum |
This genus is a mould that lacks a known sexual state and hence belongs to the Fungi Imperfecti. It is classified as a dematiaceous fungus.
Habitat/Ecology
Epicoccum is a widespread cosmopolitan saprophytic mould, most often associated with senescent and dead plant material {1781}. It is a common agent of leaf spot disease in various plants; it is also isolated from wood, paper, textiles and a variety of food, as well as on insects and human skin {816; 1056}. It is also commonly found in the soil {3964} and easily isolated from air samples {1794; 1683; 386} and occasionally found in indoor samples . The dry spores of Epicoccum are easily dispersed by wind and hygroscopic movement. In outdoor air, Epicoccum spores are more prevalent on dry, windy days, with higher counts late in the day {1781}; in urban studies, results vary greatly, ending in a classification of Epicoccum either as a minor or a major contaminant.
More details
This fungus is often found on leaf surfaces, making it a potential contributor to air spora; however, certain aerobiological studies have shown that Epicoccum is not predominant in some urban air samples even when leaf surfaces are contaminated, as demonstrated in an Oklahoma study {1281}. Similarly, a Croatian urban study found that Epicoccumwas not predominant and therefore classified the mould as a minor contaminant regrouped within the “other fungi” category {1785}.
In a study by Beaumont et al. of sampled air from a hospital rooftop in a northeastern city in the Netherlands, Epicoccumwas found to be the 8th most prevalent fungus sampled, but still represented less than 1% of the total fungus count {864}. A similar result was obtained in two major cities in Greece, namely Thessaloniki (concentration of 0.37%) {1788} and Athens (concentration of 0.3%) {1282}.
On the other hand, when measuring personal exposure to outdoor spores in an Australian city, Epicoccum was found among the most frequent taxa identified {618}. Researchers also measured the number of spores inhaled by volunteers and Epicoccum appeared to be among the most frequent.
Growth requirements
Epicoccum is a mesophilic fungus, able to grow between -3 °C and 45 °C, with optimum growth at 23-28 °C at pH 3-4.5; the thermotolerance of this fungus, which grows at 37 °C, could allow it to be a possible human pathogen {1683}. Its minimum available water requirement (Aw) is between 0.86 and 0.90 {813}, making this fungus a secondary coloniser {603}.
Water Activity : 0.86 - 0.90
Growth on building materials or indoor environment
Indoors, Epicoccum is often found in mould contaminated buildings; it can be found on gypsum boards, floors, carpet and mattress dust, as well as on house plants {1822; 3729; 1683}. In a controlled study on mould growth on wet gypsum wallboard in an indoor environment, Epicoccum did not appear as a primary coloniser, being detected only a month after immersing the building material in water {587}.
Surveys conducted to establish the prevalence and indoor concentrations of this fungus have yielded very conflicting results.
More details
In a study of concentrations and types of airborne fungi in houses in the city of Santa Fe (Argentina), Epicoccum was the third most prevalent fungus, with an occurrence of 5.74% (after Cladosporium and Alternaria) {1584}.
A study conducted in institutional buildings demonstrated that Epicoccum was able to colonise hospital ventilation and air-conditioning filter systems {386}; E. purpurascens was identified in air filters of 3 out of 7 hospitals in the eastern United States. In another study conducted during building renovation in Egypt, Epicoccum airborne spores were not among the most frequently found in the indoor air (prevalence of 0.33%) {1790}.
As Epicoccum grows often on leafs, the quality of indoor air of greenhouses and dwellings with house plants can be affected. A study demonstrated that modest numbers of undisturbed house plants contribute minimally to aeroallergen prevalence in homes, including Epicoccum, although the latter was found in about 12% of such environments {1822}. Nonetheless, especially under greenhouse conditions, plantings can harbour abundant fungal growth that may become airborne, especially when agitated directly or watered.
Laboratory section
Normal laboratory precautions should be exercised in handling cultures of this species within Biosafety Level 2 practices and containment facilities.
Colony, macroscopic morphology
Epicoccum is fast growing: on Malt extract agar or Oatmeal agar, colonies attain a diameter of at least 6 cm in 10 days. Colonies are suede-like to downy, yellow to orange, red or pink initially, becoming greenish brown to black with age. The reverse is similar, often more intensely coloured. A diffusible pigment may be produced, which turns the color of the growth medium yellow to orange or brown.
When sporulating, numerous black sporodochia (aggregates of conidiophores) are visible as black dots measuring 100 – 2 000 mm in diameter. The sporodochia may be observed macroscopically on the colony surface, appearing as tufts of hyphae with conidiophores on their surface {816; 1056}.
Microscopic morphology
The hyphae are yellow to brown. The short conidiophores, measuring 5-15 x 3-6 mm, are slightly pigmented (colourless to pale brown); they originate directly on the hyphae, mostly in clusters, repeatedly branched and terminating in more or less isodiametric conidiogenous cells. Each conidiophore produces one multicellular conidium, globose to pyriform, measuring 15-25 mm in diameter, with a funnel-shaped base and broad attachment scar when mature.
Conidia are usually present in dense masses from the clusters of conidiophores. They become dark golden brown to black and verrucose when maturing, thus obscuring the septae which divide the conidia into up to 15 cells {814; 1056}.
Specific metabolites
Organics compounds (including VOCs)
There are no reported VOCs specifically produced by Epicoccum that would be deleterious to humans or animals. Epicoccum is able to produce many secondary metabolites with potentially useful biologically active properties.
More details
For example, epicoccamides (B-D) have antiproliferative effects in leukemia cell lines {1871}; epicocone is an antioxidant {1796} and epicocconone is a natural fluorochrome whose protein affinity can be useful as a fluorescent marker {1782; 1795}.
Mycotoxins
There are no reported mycotoxins produced by Epicoccum that would be deleterious to humans or animals. Epicoccumproduces known toxic substances that are biologically active against bacteria, fungi, viruses and certain animal cells in vitro.
More details
Certain toxins, such as epicorazine B, have antifungal and antibacterial properties {3775}. Epicoccin A shows modest antimicrobial activity {3773}. Other antibiotic substances produced include epicorazine A and B, indole-3-acetonitrile and flavipin.
Adverse health reactions
Health risks associated with mould exposure in water damaged buildings are well established, especially for upper and lower respiratory tract symptoms. Epicoccum, although probably a minor contaminant, can contribute to various problems associated with indoor air quality. Health risks are essentially allergic reactions through inhalation {1802; 1683}.
Irritation and inflammation
No specific irritation or inflammation symptoms have been attributed specifically to Epicoccum but its glycoproteins are potential inflammation initiators. In vitro studies demonstrate that glycoproteins extracted from Epicoccum spores and mycelia can experimentally induce significant inflammation processes by a mannose-binding lectin (MBL) leading to the activation of the complement system {1776}.
Generally speaking, all moulds contain common substances that are irritants and promote inflammation to some degree.
More details
Some VOCs produced by moulds in the indoor setting on damp building materials are thought to contribute to different health problems, such as eye irritation, irritation of the nose and throat, and possibly to lethargy and headaches {594}.
Allergic reactions
Epicoccum is one of the important fungi responsible for inducing respiratory allergy disorders {1794; 1820} and is a significant outdoor {1780} and indoor {1790} allergen in urban communities {1813} as well as in the working place {1777}.Epicoccum allergy is prevalent worldwide: several studies have reported sensitisation to Epicoccum in 5-7% of different populations worldwide {1789} and up to 36 % of allergic patients react to skin tests performed with specific extracts {1817}. Spores of Epicoccum are recognised for generating allergens before and after germination, contrary to many other fungi which release allergens only after germination, such as Aspergillus fumigatus and Penicillium chrysogenum {935}.
Epicoccum allergy reactions include upper {1777} and lower respiratory tract disease, rhinitis, sinusitis {1790; 1781} and asthma {1780; 1817}. Elevation in outdoor Epicoccum spore concentrations may provoke or exacerbate asthma attacks in children {1780}.
More details
An association between elevated mean indoor concentrations of some fungi, including Epicoccum, and self reported respiratory health symptoms has been observed {1814}.
Atkinson et al. investigated the association between daily outdoor fungal spore concentrations and indicators of daily asthma exacerbations in a large urban population (London, UK) {1780}. Among children aged under 14, the authors found that a number of individual spores, including Epicoccum, were associated with increased attendance to hospital emergency departments; however, no such association was observed in adults.
Fungal allergy may be exacerbated by meteorological conditions, such as summertime haze episodes. Neas et al. {1810} examined the effect of such episodes in children living in Pennsylvania and reported that excessive aerosol acidity in summer and particulate pollution were acutely associated with declines in peak expiratory flow rates (PEFR) and increased incidence of cough. Airborne spore concentrations of Epicoccum, along with other fungi, were associated with these deficits in PEFR.
In the work place, Epicoccum was found to be among the dominating fungal spores inside grain storage godowns and could contribute to allergic symptoms (redness, itching, watery eyes, sneezing, cough, etc.) among the workers {1777}.
In Toronto (Canada), Tarlo et al. quantified and identified airborne fungal species in the homes of patients with allergic rhinitis or asthma; thereafter, using skin-prick tests, authors found that 36% of tested individuals reacted positively toEpicoccum purpurascens. A similar experiment with outpatients from an allergology department in the Netherlands revealed a positive skin test in 4.9% of patients tested {864}. A study investigating patients with asthma as well as people in the community detected 21.6% positive skin tests to Epicoccum in intensive care unit patients, 20% in subjects admitted to hospitals and 2% in the community {1806}.
In a study characterising skin test reaction frequencies and reactivity to many aeroallergens in a population of patients with allergic disease in Missouri, Chapman et al. found that among the fungi group, one fourth (25%) of all patients were positive to Epicoccum, supporting the reports placing this genus as a dominant airborne mould {1820}.
In occupants of water-damaged buildings, researchers simultaneously measured IgA, IgE, IgG and IgM antibody levels against the most common moulds and their mycotoxins in order to investigate whether other allergic reactions, in addition to Type I allergy and asthma, were induced by these exposures {116}. Antibodies (IgM, IgG or IgA) were found to be significantly elevated against many of the tested fungi, but not against Epicoccum, even if experimental studies had shown the immunogenic properties of this fungus {1802}.
Allergic components and mechanism
Culture filtrates from Epicoccum purpurascens (nigrum) display protein compounds reacting with IgG and IgE rabbit antibodies, revealing its allergenic and immunogenic nature {1802}. Crude fungal extracts of Epicoccum contain a large number of major/minor allergenic proteins {1813} which are not yet all characterised.
A major glycoprotein allergen, Epi p 1, has been purified {1794} and shows extensive cross-reactivity with other species, such as Alternaria alternata, Aspergillus fumigatus and Chrysogenum herbarum. This allergen protease may induce histamine release in patients allergic to Epicoccum {1789}.
Hypersensitivity pneumonitis
Type III hypersensitivity pneumonitis (HP) due to Epicoccum has been reported in one case of indoor exposure: two young siblings exposed to an unventilated basement shower developed a serologically confirmed Epicoccum HP{1683}.
Toxic effects (mycotoxicosis)
No human or animal mycotoxicosis associated to Epicoccum has been reported.
Infections and colonisations
Epicoccum is often been said to be non infectious and when it is occasionally isolated from clinical samples, it is presumed to be a contaminant {813; 816}. Only one reported case mentions a fatal bloodborne infection in a severely immunosuppressed allogenenic hematopoietic stem cell transplant (HSCT) recipient, where the possible identified agent was Epicoccum {1792}.
More details
Sadfar et al. performed a retrospective analysis to evaluate the clinical significance of blood culture isolates of non-Candida fungal species found in severely immunosuppressed patients. Out of the 48 patients studied, 5 patient deaths were attributed to fungemia that occurred due to haematogenous mycosis, one of which was attributable to Epicoccum.According to this study, severely immunosuppressed individuals, such as those with haematologic malignancies, recipients of hematopoietic stem cell transplantation and patients receiving cytotoxic therapy for postransplantation complications, remain a population at risk for fungal infections, including Epicoccum {1792}.
Virulence factors
As no confirmed Epicoccum infections have been reported, it is presumed that this fungus possesses no particular virulence factor.
However, the thermotolerance of this fungus, which can grow at 37 °C, allows it to be a possible human pathogen {1683}.
Specific settings
Nosocomial infections
Epicoccum has been found in the hospital setting {386}. However, no confirmed Epicoccum nosocomial infection has been reported.
More details
A study demonstrated that Epicoccum can colonise hospital ventilating and air-conditioning filters {386}: E. purpurascenswas identified in the air filters of 3 out of 7 hospitals studied in the eastern United States.
Occupational diseases
Epicoccum has been reported in certain occupational environments, particularly where plant material and grain are handled {1822; 1777}. Because of the well known allergenic properties of Epicoccum, such exposures could lead to allergic responses and hypersensitivity reactions; in one study, this exposure was associated with restrictive, obstructive and combined types of respiratory impairments among grain storage depot workers {1777}. However Type III hypersensitivity pneumonitis has not been reported in occupational settings.
Diagnostic tools
Cultures
Cultures of sinus secretions may help in confirming Epicoccum as the agent of allergic fungal sinusitis in certain cases {1776; 719}.
Observation of fungal elements by direct examination of these same secretions is usually considered a confirmation a fungal allergic sinusitis.
Histopathology
No infectious histopathological data have been reported; no confirmed Epicoccum infection has been reported.
Specific histological staining of sinus secretions has shown the presence of antibodies on the surface of fungal fragments present in these secretions.
These staining methods could be useful in confirming Epicoccum as the underlying agent in sinusitis aetiology.
Immunodiagnosis
Both in vivo and in vitro testing are commercially available and may be useful in associating an allergic reaction to Epicoccum exposure.
More details
Epicoccum allergen preparations for use in vivo and/or in vitro are commercially available either as single allergens or as (pooled antigens, antigen mixes){3284; 581}.
The Epicoccum allergen extracts registered with the American «Biological Products Deviation Reporting» surveillance program of the Federal Drug Administration (FDA) {3285} are as follows :
- GJ50 - Epicoccum nigrum
- GJ51 - Epicoccum purpurascens
- GJ52 - Epicoccum sp.
| Test | IgE | IgG | Antigens | Other |
|---|---|---|---|---|
| Skin Tests | X | |||
| RAST-IgE | X | |||
| RAST-IgG | X | |||
| ELISA-ELIFA | ||||
| Immunodiffusion | ||||
| Immunofluorescence | ||||
| Complement fixation | ||||
| PCR | ||||
| Other |
Bibliography
- 116. Vojdani, A., Campbell, A. W., Kashanian, A., and Vojdani, E. (2003). Antibodies against molds and mycotoxins following exposure to toxigenic fungi in a water-damaged building. Arch Environ Health. 58[6], 324-336.
- 386. Simmons, R. B., Price, D. L., Noble, J. A., Crow, S. A., and Ahearn, D. G. (1997). Fungal colonization of air filters from hospitals. Am Ind.Hyg.Assoc.J. 58[12], 900-904.
- 581. Pharmacia Diagnostics AB. (2007). Allergy & autoimmunity. Diagnostics product catalogue 2007. internet , 1-48. Pharmacia.
- 587. Krause, M., Geer, W., Swenson, L., Fallah, P., and Robbins, C. (2006). Controlled study of mold growth and cleaning procedure on treated and untreated wet gypsum wallboard in an indoor environment. J Occup.Environ Hyg. 3[8], 435-441.
- 594. Claeson, A. S., Levin, J. O., Blomquist, G., and Sunesson, A. L. (2002). Volatile metabolites from microorganisms grown on humid building materials and synthetic media. J Environ Monit. 4[5], 667-672.
- 603. Nielsen, K. F., Gravesen, S., Nielsen, P. A., Andersen, B., Thrane, U., and Frisvad, J. C. (1999). Production of mycotoxins on artificially and naturally infested building materials. Mycopathologia. 145[1], 43-56.
- 618. Green, B. J., O'meara, T., Sercombe, J., and Tovey, E. (2006). Measurement of personal exposure to outdoor aeromycota in northern New South Wales, Australia. Ann Agric.Environ Med. 13[2], 225-234.
- 719. Noble, J. A., Crow, S. A., Ahearn, D. G., and Kuhn, F. A. (1997). Allergic fungal sinusitis in the southeastern USA: involvement of a new agent Epicoccum nigrum Ehrenb. ex Schlecht. 1824. J Med Vet.Mycol. 35[6], 405-409.
- 813. EMLAB. (2007). Environmental Microbiology Laboratory, Inc. (EMLab): An index of some commonly encountered fungal genera.
- 814. Ellis, D. (2007). Mycology online. University of Adelaide . School of molecular & biomedical science. The University of Adelaide.
- 816. Patterson, T. F., McGinnis, M. R., and ed. (2009). The fungi :description. Site Doctor Fungus . Mycoses Study Group.
- 864. Beaumont, F., Kauffman, H. F., de Monchy, J. G., Sluiter, H. J., and de Vries, K. (1985). Volumetric aerobiological survey of conidial fungi in the North-East Netherlands. II. Comparison of aerobiological data and skin tests with mould extracts in an asthmatic population. Allergy. 40[3], 181-186.
- 935. Green, B. J., Mitakakis, T. Z., and Tovey, E. R. (2003). Allergen detection from 11 fungal species before and after germination. J Allergy Clin Immunol. 111[2], 285-289.
- 1056. Samson, RA, Hoekstra, ES, and Frisvad, JC. (2004). Introduction to food and airbone fungi. 7th, -389 p. Baarn, Centralalbureau voor Schimmellcultures, Institute of the Royal Netherlands Academy of Arts and Sciences.
- 1281. Levetin, E. and Dorsey, K. (2006). Contribution of leaf surface fungi to the air spora. Aerobiologia 22[1], 3-12.
- 1282. Pyrri, I. and Kapsanaki-Gotsi, E. (2007). A comparative study on the airbone fungi in Athens, Greece, by viable and non-viable sampling methods. Aerobiologia 23, 3-15.
- 1584. Basilico, Mde L., Chiericatti, C., Aringoli, E. E., Althaus, R. L., and Basilico, J. C. (2007). Influence of environmental factors on airborne fungi in houses of Santa Fe City, Argentina. Sci Total Environ. 376[1-3], 143-150.
- 1683. Hogan, M. B., Patterson, R., Pore, R. S., Corder, W. T., and Wilson, N. W. (1996). Basement shower hypersensitivity pneumonitis secondary to Epicoccum nigrum. Chest. 110[3], 854-856.
- 1776. Kukreja, N., Arora, N., Singh, B. P., Das, H. R., and Sridhara, S. (2007). Role of Glycoproteins Isolated from Epicoccum purpurascens in Host-Pathogen Interaction. Pathobiology. 74[3], 186-192.
- 1777. Chattopadhyay, B. P., Das, S., Adhikari, A., and Alam, J. (2007). Exposure to varying concentration of fungal spores in grain storage godowns and its effect on the respiratory function status among the workers. Ind Health. 45[3], 449-461.
- 1780. Atkinson, R. W., Strachan, D. P., Anderson, H. R., Hajat, S., and Emberlin, J. (2006). Temporal associations between daily counts of fungal spores and asthma exacerbations. Occup Environ Med. 63[9], 580-590.
- 1781. Weber, R. W. (2006). On the cover: Epicoccum pupurascens. Ann Allergy Asthma Immunol. 96[1], A6.
- 1782. Choi, H. Y., Veal, D. A., and Karuso, P. (2006). Epicocconone, a new cell-permeable long Stokes' shift fluorescent stain for live cell imaging and multiplexing. J Fluoresc. 16[4], 475-482.
- 1785. Peternel, R., Culig, J., and Hrga, I. (2004). Atmospheric concentrations of Cladosporium spp. and Alternaria spp. spores in Zagreb (Croatia) and effects of some meteorological factors. Ann Agric Environ Med. 11[2], 303-307.
- 1788. Gioulekas, D., Damialis, A., Papakosta, D., Spieksma, F., Giouleka, P., and Patakas, D. (2004). Allergenic fungi spore records (15 years) and sensitization in patients with respiratory allergy in Thessaloniki-Greece. J Investig.Allergol.Clin Immunol. 14[3], 225-231.
- 1789. Bisht, V., Arora, N., Singh, B. P., Pasha, S., Gaur, S. N., and Sridhara, S. (2004). Epi p 1, an allergenic glycoprotein of Epicoccum purpurascens is a serine protease. FEMS Immunol.Med Microbiol. 42[2], 205-211.
- 1790. Abdel Hameed, A. A., Yasser, I. H., and Khoder, I. M. (2004). Indoor air quality during renovation actions: a case study. J Environ Monit. 6[9], 740-744.
- 1792. Safdar, A., Singhal, S., and Mehta, J. (2004). Clinical significance of non-Candida fungal blood isolation in patients undergoing high-risk allogeneic hematopoietic stem cell transplantation (1993-2001). Cancer. 100[11], 2456-2461.
- 1794. Bisht, V., Arora, N., Singh, B. P., Gaur, S. N., and Sridhara, S. (2004). Purification and characterization of a major cross-reactive allergen from Epicoccum purpurascens. Int Arch Allergy Immunol. 133[3], 217-224.
- 1795. Mackintosh, J. A., Choi, H. Y., Bae, S. H., Veal, D. A., Bell, P. J., Ferrari, B. C., Van Dyk, D. D., Verrills, N. M., Paik, Y. K., and Karuso, P. (2003). A fluorescent natural product for ultra sensitive detection of proteins in one-dimensional and two-dimensional gel electrophoresis. Proteomics. 3[12], 2273-2288.
- 1796. Abdel-Lateff, A., Fisch, K. M., Wright, A. D., and Konig, G. M. (2003). A new antioxidant isobenzofuranone derivative from the algicolous marine fungus Epicoccum sp. Planta Med. 69[9], 831-834.
- 1802. Bisht, V., Singh, B. P., Kumar, R., Arora, N., and Sridhara, S. (2002). Culture filtrate antigens and allergens of Epicoccum nigrum cultivated in modified semi-synthetic medium. Med Microbiol Immunol. 191[1], 11-15.
- 1806. Black, P. N., Udy, A. A., and Brodie, S. M. (2000). Sensitivity to fungal allergens is a risk factor for life-threatening asthma. Allergy. 55[5], 501-504.
- 1810. Neas, L. M., Dockery, D. W., Burge, H., Koutrakis, P., and Speizer, F. E. (1996). Fungus spores, air pollutants, and other determinants of peak expiratory flow rate in children. Am J Epidemiol. 143[8], 797-807.
- 1813. Dixit, A. B., Lewis, W. H., and Wedner, H. J. (1992). The allergens of Epicoccum nigrum Link. I. Identification of the allergens by immunoblotting. J Allergy Clin Immunol. 90[1], 11-20.
- 1814. Su, H. J., Rotnitzky, A., Burge, H. A., and Spengler, J. D. (1992). Examination of fungi in domestic interiors by using factor analysis: correlations and associations with home factors. Appl Environ Microbiol. 58[1], 181-186.
- 1817. Tarlo, S. M., Fradkin, A., and Tobin, R. S. (1988). Skin testing with extracts of fungal species derived from the homes of allergy clinic patients in Toronto, Canada. Clin Allergy. 18[1], 45-52.
- 1820. Chapman, J. A. and Williams, S. (1984). Aeroallergens of the southeast Missouri area: a report of skin test frequencies and air sampling data. Ann Allergy. 52[6], 411-418.
- 1822. Burge, H. A., Solomon, W. R., and Muilenberg, M. L. (1982). Evaluation of indoor plantings as allergen exposure sources. J Allergy Clin Immunol. 70[2], 101-108.
- 1871. Wangun, H. V., Dahse, H. M., and Hertweck, C. (2007). Epicoccamides B-D, glycosylated tetramic acid derivatives from an Epicoccum sp. associated with the tree fungus Pholiota squarrosa. J Nat.Prod. 70[11], 1800-1803.
- 3284. Hollister-Stier Laboratories. (2009). Allergenic extracts : Molds. Hollister-Stier Laboratories .
- 3285. Federal Drug Administration (FDA). (2008). Biological products deviation reporting (BPDR). Non-blood product codes. 3-29-2009.
- 3318. UniProt Consortium. (2009). Taxonomy : fungi metazoa group. Site de UniProt . 4-6-2009.
- 3729. Flannigan, B., Samson, R. A., and Miller, J. D. (2002). Microorganisms in home and indoor work environments: diversity, health impacts, investigation and control. -504 p. CRC Press.
- 3773. Zhang, Y., Liu, S., Che, Y., and Liu, X. (2007). Epicoccins A-D, epipolythiodioxopiperazines from a Cordyceps-colonizing isolate of Epicoccum nigrum. J Nat.Prod. 70[9], 1522-1525.
- 3775. Mallea, M., Pesando, D., Bernard, P., and Khoulalene, B. (1991). Comparison between antifungal and antibacterial activities of several strains of Epicoccum purpurascens from the Mediterranean area. Mycopathologia. 115[2], 83-88.
- 3964. Domsch, K. H., Gams, W., and Anderson, T.-H. (1993). Compendium of soil fungi. [1-2], -1264. IHW Verlag.