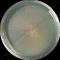
Chaetomium spp.
Basics
Taxonomy
| Kingdom | Fungi | Order | Sordariales |
| Phylum | Ascomycota | Family | Chaetomiaceae |
| Class | Euascomycetes | Genus | Chaetomium |
The genus Chaetomium comprises between 80 and 100 species, depending on the consulted documents: taxonomic data vary greatly for this genus {3318}. Chaetomium globosum is the best known and studied species {767}. Some of the most common ones are Chaetomium atrobrunneum, Chaetomium funicola, Chaetomium globosum, and Chaetomium strumarium.
Habitat/Ecology
Chaetomium are common fungal species with a worldwide ubiquitous distribution and are widespread in soil and on decaying plant materials {724, 741} but spore concentrations in outdoor air are not very high {1175, 3314}. Indoors, these fungi live on cellulose, and are found on wood, compost, sheet rock, straw, and similar materials. It is also known as a soft-rot fungus for softwood and hardwood timber {724}.
Chaetomium are also found indoors on a variety of substrates containing cellulose, including document archives, wallpaper, textiles and construction materials {989}.
More details
They have even been isolated from degraded polyimide coatings, showing extensive colonisation, and first studies indicate that this fungus may cause breakdown of plastics and polymers {3358}.
In cold climates, this fungus can take as long as three weeks to mature. Spores are formed inside fruiting bodies named perithecia. At maturity or by mechanical disturbance, the perithecia break up, and spores are forced out and spread by wind, insects and water splash.
Growth requirements
Some Chaetomium grow well between 16 and 25°C, and most species grow best between 25 and 35°C. A few species being thermotolerant or thermophilic {1872}; in fact, those that have been reported to cause invasive human diseases grow also well between 35 and 37°C {737}.
In fact, according to the optimal growth temperature when cultivated on Malt Agar with 2% yeast extract, one can distinguish several groups of Chaetomium: mesophilic (15 35°C), semi-mesophilic (15-37°C), microthermophilic (15-40°C), thermotolerant (15 45°C) and thermophilic (25-55°C) {3363}.
The thermal point of mortality of the species C. globosum is of 55-57°C. On the other hand, ascospores are even more resistant to environmental conditions: they can survive at 60°C for 60 minutes {767}. In vitro, on Sabouraud Agar medium, they show a slight heat resistance, surviving at 60°C for 60 minutes, but not at 70°C for 10 minutes as other soilborne microfungi can {2497}. Their ascospores may germinate at temperatures in the 4-10°C to 38°C range, optimally at 24-28°C {989}.
C. globosum will grow best at a pH between 7,1 and 10,4, but may also grow at pH of 3,5 11 {989}. Chaetomium sp. requires a water activity (Aw – available water) higher than 0,90 for growth {876, Andersen, B., 2000}, optimally 0,94 {989, 724}. Because of this requirement, Chaetomium sp. is regarded as a tertiary coloniser, like others high Awfungi such asStachybotrys, Alternaria, Fusarium and Ulocladium {603}.
Water Activity: Aw = 0.91-0.94
Growth on building materials or indoor environment
Chaetomium spp. grow well on most cellulose containing building materials in water damaged buildings {3289}. These cellulolytic fungi are widespread and very commonly found on damp sheetrock paper. Several Chaetomium species are very common in indoor environments: C. elatum, C. globosum and C. murorum {1872}.
More details
Assessment studies done inside homes and public buildings, by air {1527, 1528} and surface {1175} and settled dust sampling {550}, have found Chaetomium prevalent under many latitudes and climates {635, 199, 1175}.
In indoor environment, isolates of Chaetomium were reported found in house dust {1829}, growing on damp building materials containing cellulose-based materials (such as wood, wallpaper and cardboard) affected by leaking water; Chaetomium is reported as one of the most frequent fungal genus in those conditions, often ranking in third position afterPenicillium spp. and Aspergillus spp. {767, 605, 876, 550, 807, 1527}.
On artificially infested building materials, Chaetomium’s development is very fast, covering the surface with substantial growth after two weeks {603}. However, since the spores are cemented together by mucilage and are also trapped by hairs, few become airborne until the mould has completely dried out or is mechanically disturbed during renovations or mould remediation. It is, therefore, not uncommon to find low Chaetomium spore counts in pre-remediation air samples and relatively higher counts in post-remediation samples {3313}.
When dealing with indoor contamination, in particular when dealing with cases of sick building syndrome related fungi, fumigation treatment with chloride dioxide has some fungicidal effects on Chaetomium, but strains of this species appeared to be more resistant than Stachybotrys chartarum and Penicillium chrysogenum {732}.
Laboratory section
Normal laboratory precautions should be exercised in handling cultures of this species within Biosafety Level 2 practices and containment facilities.
Colony, macroscopic morphology
The surface of the colony is spreading, cottony, usually white, becoming tannish gray or greyish olive with age. The reverse in usually orange-tan tinted with red but may be brown to black {412}. On Malt Agar medium, colonies have a granular aspect, green-dark with black reverse. On Czapek, colonies are translucent white with a colourless reverse. On CYA medium, they are filamentous, granular, greyish in the center, green towards the outskirt. The reverse is dark-red in the center, green-black on outside {989}. Cultures have a strong “musty” or “mildew” odour.
Chaetomium grows and sporulates on general fungal media. Growth is quite rapid {415}, colonies on Oatmeal Agar at 24°C attain a diameter of 5.0 7.0 cm in 10 days. Chaetomium may need 8-20 days for fruiting body production and sporulation: at maturity, the fungal mat consists of a dense layer of fruiting bodies {724}.
Microscopic morphology
The thallus is made up of septate hyphae, hyaline to light brown in colour. Among the septate hyphae, large flask-shaped fruiting bodies (perithecia) are easily seen (100-150 x 110-225 µm) on most media: they are best seen on Potato Dextrose Agar (PDA) on which they appear as dark-brown to blackish, globose to ovoid (egg-shaped) opaque structures surrounded with thick hair-like hyphal filaments called setae. These perithecia contain multiple sac-like structures (asci), each enclosing spores (ascospores). The dark setae can take a variety of forms, depending upon the species. They can be septate, unbranched, flexuous or even coiled, pigmented and rough-walled. Asci are stalked, club-shaped, containing 4 or 8 spores; the ascospores readily observed coming out of the perithecium, are brown, oval or have a distinctive lemon-shaped (9-11 x 7 8.5 µm) but may occur in a variety of sizes, shapes, and colours. The ascospores are very resistant to dry conditions and UV irradiation {2207, 412, 724}.
Specific metabolites
Organics compounds (including VOCs)
In pure culture, Chaetomium species produce many secondary metabolites and mycotoxins {876}; compounds such as enzymes, ergosterol, alkaloids {2522}, antibiotics (chaetocins, chaetomin, cochliodinol), and antifungal compounds have been often reported {767, 1772, 876, 1741}. Some of the other metabolites reported are: heptelidic acid, alternariol monomethyl ether, chaetomanone, chrysophanol, cochliodinol, and cytochalasane.
In a study of strains of indoor mouldy building provenance, exometabolites of Chaetomium were found active in vitro (6/14 strains) and showed some ciliostatic activity {767}:
However, the effects of Chaetomium mVOCs on humans exposed to contaminated building materials have not yet been studied.
Mycotoxins
Species of Chaetomium are known to produce many potent mycotoxins. Some of these are: chaetoglobosins, chaetoatrosin, chaetomanone, chaetochromins (A to D), chaetocin, chaetomin, cochliodinols, mollicellins and sterigmatocystins and O methylsterigmatocystin {746, 800}. Chaetochromins have reported as teratogen {1767}.The main toxins produced are chaetoglobosins (A to K) {727}; new chaetoglobosins (Q,R and T) have recently been added to those previously characterized {1744}.
Some Chaetomium species have been reported to produce sterigmatocystin which is a potent carcinogen {876}. Several species of Chaetomium produce mycotoxins when growing on vegetable matter and sometimes on building materials.
More details
Chaetomium globosum, C. mollipilium, C. rectum, and C. subaffine as well as C. cochliodes are known to produce chaetoglobosins. From cultures of C. thielavioideum, chaetocin, sterigmatocystin and O-methylsterigmatocystin were isolated {797}.
Chaetominine, a cytotoxic alkaloid, was characterized from a strain of Chaetomium sp. {726}. New metabolites are currently discovered, following screening of different strains; among these, immunosuppressive chetomin-related metabolites were discovered {1745}.
C. globosum produces high quantities of mycotoxins, especially chaetoglobosins A and C, even when growing on gypsum board {603, 767, 800}:even relatively low levels of these compounds have been shown to be lethal for various tissue culture cell lines {3289}. Species C. mollicelum and C. globosum produce mutagenic products called mollicellins, (C, D, E, and G){767, 1772, 1395, 727}.
Cytotoxic orsellinic acid esters (globosumones A-C) have been isolated from an endophytic strain of C. globosum {1739}.
Some studies have been conducted on the production of mycotoxins by Chaetomium spp. in the indoor environment {1395}. Chaetomium globosum, the most common species within this genus, produces chaetoglobosins A and C when cultured on building materials {3289}. In this study, out of 30 C. globosum isolates from water-damaged buildings cultured on OA media for 4 weeks, 16 produced detectable amounts of chaetoglobosin A, and every isolate produced chaetoglobosin C.
Airway toxic endometabolites and exometabolites, extractable from house dust with chloroform, have been linked to the presence of Chaetomium isolated from the same house dust {550, 767}.
Adverse health reactions
Health risks associated with mould exposure in water-damaged buildings are well established, especially for upper and lower respiratory tract symptoms. Chaetomium spp. are among the most prevalent moulds in this setting; Chaetomium could thus significantly contribute to different indoor air problems.
Irritation and inflammation
No report has been made concerning inflammation reactions in humans specifically due to Chaetomium exposure.
Nonetheless, this genus does produce many potentially irritant substances that could contribute to the reported health effects linked to the exposure to a mouldy environment. In general, a number of organic compounds of fungal origin, including volatile organic compounds (mVOCs), have been identified in indoor air in damp buildings: these are thought to contribute to different indoor air quality problems. Most of identified metabolites are non-reactive and found in low concentrations in the indoor air {594}.
Allergic reactions
Chaetomium sp. is reported to be allergenic {741}. Some species are linked to Type I allergies, hay fever and asthma {2342, 3095} as well as to allergic sinusitis. In one study of atopic patients, 7% of the subjects had positive skin tests for C. globosum {2255}.
More details
Even if Chaetomium, especially C. globosum, sensitisation is fairly prevalent, hypersensitivity reactions to the Chaetomium genus, in particular IgE-mediated reactions, have not been well studied. In spite of the fact that Chaetomium species produce airborne spores often found in spore counts, it appears that organisms in this genus seldom induce IgE-mediated reactions in sensitised individuals: It is not clear whether Chaetomium has an actual low allergenic potential or if this impression is the result of the lack of study of this fungus as an allergen {3364}.
Chaetomium has been associated with cases of asthma. A species of Chaetomium, C. umbratile, was reported isolated from house dust samples, in asthmatic patients’ dwellings {1829}. In a Brazilian study, evaluating sensitisation in patients with asthma and/or allergic rhinitis to 42 airborne fungi using skin specific IgE tests, 15/201 subjects were shown to be sensitised to Chaetomium allergens {3362}. In an other study, the moulds Chaetomium globosum, Aspergillus fumigatus, and the Eurotium group were the primary species found in the NC homes of asthmatic children {1527}.
In the differential diagnosis between allergic and non-allergic asthma, the addition of Chaetomium allergens to the standard battery of skin tests has proven to be useful, suggesting that Chaetomium allergy is under diagnosed {1759}.
Chaetomium globosum was amongst the fungi associated with allergic sinusitis in a study of teachers exposed to a mouldy environment. One study found an association between sinusitis and elevated mould-specific IgG levels for many species, including Chaetomium globosum {199}. The same Chaetomium exposure may also play a role in the human paranasal sinus infection or colonisation: in one case, histological examination following infundibulectomy showed necrotic material with hyphae of A. fumigatus and perithecia of Chaetomium sp. {1754}.
Allergic components and mechanism
No purified allergen fractions have yet been characterised.
Hypersensitivity pneumonitis
Type III hypersensitivity pneumonitides (HP) due specifically to Chaetomium have not yet been reported.
More details
However, complex fungal exposures are known to be associated with HP. One example is the complex ecosystem that can be found in a contaminated humidifier system: bacteria such as Klebsiella species and many moulds such as Aureobasidium, Chaetomium, Pullularia, Cephalosporium, Curvularia, and Penicillium species. In this particular instance, we do not know the extent of the contribution of Chaetomium antigens to the humidifier lung syndrome. Even in the context of a specific exposure, there can be several potential antigens that might be triggering the inflammatory lung disease {3360}.
Toxic effects (mycotoxicosis)
Chaetomium produce many highly toxic compounds under given sets of growth conditions. Relatively low levels of these compounds have been shown to be lethal to various tissue culture cell lines {1153, 746, 800}.
Some toxicity studies have been conducted on animals, but Chaetomium mycotoxicosis in humans has not been well studied. However, studies have shown contaminated cereals to be extremely toxic, even lethal, when fed to animals {1775, 1771, 1769,}.
Crude extracts of Chaetomium, studied in mice, have shown spleen, liver and kidney toxicity {1771}; in this model, the extracts have been associated with hemoglobinuria and hemorrhagic enteritis.
More details
Toxicity of C. globosum, using strains isolated from corn, was tested by feeding animals. The results indicate that isolates of this species, when grown on corn, are remarkably toxic to rats but harmless to swine. In this study, premortem symptoms lesions included hemoglobinuria and hemorrhagic enteritis {1775}.
A similar experiment was done with mice receiving intraperitoneally crude toxin from strains collected from maize and wheat fields. Chaetomium was found to be quite toxic, damaging kidneys, spleen and liver. In fact, in this particular study, among the different fungal contaminants showing 1+ toxicity, the Chaetomium spp. extracts were found to be the most toxic, damaging all 3 organs and causing 12.5% of mortality. {1771}. An other experiment using Chaetomium sp. from contaminated corn as a feed ingredient caused 100% mortality in broiler chicks {1769}.
Chaetochromin, a polyphenolic mycotoxin produced by Chaetomium sp., has proven to be teratogenic to mice embryos when administered orally to the mother {1767}.
On human cell lines, cytochalasin B, one of the many Chaetomium toxins, has proven to be a remarkably specific and potent inhibitor of D-glucose transport in human erythrocytes: this inhibition mechanism is explained to be a kinetically competition type {3361}.
Because of the high toxicity of ingested or injected Chaetomium extracts in animals and given the few conclusive studies on human cell lines, there are some concerns about the potential effects of indoor Chaetomium exposure. Some authors suggest that Chaetomium mycotoxins present indoors, could pose a risk to exposed occupants. The possible toxic effect of Chaetomium strains on the respiratory tract should not be underestimated in occupants of damp mouldy buildings {767} and long-term chronic exposure studies should be undertaken to assess correctly the health effects due to Chaetomium inhaled mycotoxins {87, 800}.
Infections and colonisations
Cases of confirmed human Chaetomium infection are rare. Chaetomium are among the fungi causing infections often referred to as phaeohyphomycosis or hyalohyphomycosis. Brain abscess, peritonitis, cutaneous and subcutaneous lesions may develop. Onychomycosis of the toenails or fingernails may be exceptionally caused by Chaetomium sp. in people with normal immunity {1760}.
The full spectrum of Chaetomium mycoses includes onychomycosis, sinusitis, empyema, pneumonia and fatal disseminated cerebral disease in immunocompromised hosts and intravenous drug users.
Several reports have been published, implicating species of Chaetomium as opportunistic infectious pathogens; in a case review, C. globosum was the most common species being isolated in, at least, nine clinical cases of infection {1755}. As the diagnosis of pulmonary fungal infections is difficult, in absence of a cultural isolate, some cases may have been falsely attributed to Aspergillus, both on clinical symptoms and even on histopathology exams {1743}.
More details
Respiratory infections have been reported. A first case of a pneumonia caused by C. globosum was reported in a patient with acute myeloblastic leukemia {740}. An other case was reported in a person with a history of asthma and chronic bronchiectasis, who developed a right-middle-lobe syndrome in his lung, following infection with a new strain, C. perlucidum {737}.
A case of pneumonia caused by Chaetomium globosum was diagnosed in a leukemic patient: the computed tomography chest scan revealed cavitating lesions characteristic of an invasive fungal infection in the right upper lobe, and a right lobectomy was performed. Histology demonstrated branching hyphae invading blood vessels that were “consistent with Aspergillus. This case was however confirmed by PCR as being caused by C. globosum {1743}.
Chaetomium was isolated from the bronchoalveolar lavage of an hospitalized patient nursed in a room where three patients colonised with this fungus had been housed before; the air filter system was subsequently found to be contaminated with Chaetomium {740}.
A paranasal sinuses infection, diagnosed in a women, revealed necrotic material with hyphae of Aspergillus fumigatus and perithecia of Chaetomium sp.; authors report that growth of Chaetomium can be stimulated in the presence of A. fumigatus {1754, 1753}.
Cerebral infections have been reported in patients presenting different risk factors. Three cases of fatal cerebral mycosis caused by C. strumarium have been reported in males with prior histories of intravenous drug use. These infections were most likely acquired by direct intravenous injection of the fungus and it’s subsequent spread; it was suggested that brain tissue provides an environment for rapid growth and proliferation of this fungus {741}.
A case of fatal invasive mycosis {737} has been reported in a patient with acute myelogenous leukemia: this infection was caused by a new species, C. perlucidum {737}. Chaetomium atrobrunneum, a new pathogen, has also been associated with cerebral infections in the immunocompromised hosts {1749}.
Cutaneous and subcutaneous phaeohyphomycosis were reported in people with non clinical signs of immunodeficiency {728, 1766}. Although onychomycosis is recognized to be caused by Chaetomium, there have been only few credible descriptions of this infection caused by this fungal genus {1736}. This onychomycosis can be successfully treated with itraconazole {729}.
Virulence factors
No particular virulence factors have been reported.
More details
However, when pathologic changes (consolidated lung lesions and histologic lesions) were studied following tracheal inoculation of goats, C. globosum seems to be the most infectious of the Chaetomium, ranking third of the seven fungi; C. globosum ranked third after Mucor ramosissmus and Trichoderma viride {902}.
Specific settings
Nosocomial infections
Very few Chaetomium spp. infections have been reported as possibly acquired in the hospital setting.
The genus Chaetomium is mentioned as part of the possible causative agents of nosocomial mycoses among the emerging fungal pathogens posing a risk for immunocompromised patients {1747, 2123}. However, events involving Chaetomium are hardly ever reported.
More details
In one instance, four bone marrow transplant recipients, who consecutively occupying the same room in an Oncology-Haematology Special Care Unit (OHSCU), became colonised with Chaetomium. Environmental cultures revealed Chaetomium contamination of the OHSCU air handling system, including the HEPA (high-efficiency particulate air) filters {1765}. At the time of Chaetomium colonisation, all patients were febrile, two had transient new infiltrates on chest X-rays, and three were receiving amphotericin B therapy.
Receiving antimicrobial agents or chemotherapy, immunosuppression, organ transplantation, neutropenia and presence of indwelling intravascular catheter are known risk factors for fungal infections and could be factors permitting Chaetomium infections in the hospital setting and during the peri-hospitalization period {1735}. Some of them can be a cause of devastating complications following fungal infections {740}. However, Chaetomium present in the hospital environment have been reported only in four occasions and only in immunocompromised subjects {740}.
Invasive and life-threatening Chaetomium infections have occurred in association with drug use (through direct inoculation), but the majority have involved patients with haematologic malignancy {1770} or immunosuppression secondary to a bone marrow transplantation (organ transplantation), a condition which appeared to be the most frequent risk factor {737, 1734, 1750, 1751, 1765}.
Occupational diseases
Type III hypersensitivity pneumonitides due to Chaetomium spp. are not known in any particular occupational settings. (See adverse health reactions section.)
Species of Chaetomium being clearly allergenic and growing readily in decaying plant material and compost, this fungus could represent a risk for workers exposed to such contaminated material.
Diagnostic tools
Cultures
No specific report of the diagnostic value of cultures or their success in cases of deep sited infections. (See laboratory section for possible culture results.)
Histopathology
The histological presentation of a deep-sited infection due to Chaetomium is typically that of an opportunistic fungal hyphal infection.
Immunochemical staining of lung sections from a pneumonia case, involving Chaetomium globosum, revealed branching hyphae in the tissue sections (see figure 1) {740}. Molecular confirmation of this invasive infection, by DNA amplification, has been obtained {1743}.
In one case of fatal cerebral mycosis, the section of brain, stained with Gomori methenamine-silver, showed branched septate hyphae, often with slight swellings (see figure 2). Many hyphae had grown around the blood vessels. The section from the deep white matter showed necrosis and dense acute inflammation and was positive for fungal elements by hematoxylin and eosin staining. A Masson-Fontana stain was only faintly positive. Acid-fast bacillus and Gram stain were negative {3317}.
Immunodiagnosis
| Test | IgE | IgG | Antigens | Other |
|---|---|---|---|---|
| Skin Tests | X | |||
| RAST-IgE | X | |||
| RAST-IgG | X | |||
| ELISA-ELIFA | ||||
| Immunodiffusion | ||||
| Immunofluorescence | Experimental | |||
| Complement fixation | ||||
| PCR | Experimental | |||
| Other |
More details
Les préparations d’allergènes les plus communes pour l’usage in vivo ou in vitro, qui sont disponibles sur le marché, sont le Chaetomium globosum et un « pool » d’espèces de Chaetomium {581, 3284}.
Les allergènes de Chaetomium répertoriés par la FDA sont les suivants :
GJ34 - Chaetomium globosum GJ35 - Chaetomium indicum GJ36 - Chaetomium olivaceum GJ37 - Chaetomium sp.
Bibliography
- 87. Jarvis, B. B. and Miller, J. D. (2005). Mycotoxins as harmful indoor air contaminants. Appl.Microbiol Biotechnol. 66[4], 367-372.
- 199. Patovirta, R. L., Reiman, M., Husman, T., Haverinen, U., Toivola, M., and Nevalainen, A. (2003). Mould specific IgG antibodies connected with sinusitis in teachers of mould damaged school: a two-year follow-up study. Int J Occup.Med Environ Health. 16[3], 221-230.
- 412. Larone, D H. (1987). Medically important fungi. A guide to identification. 2nd edition, -230 p. New York - Amsterdam - London, Elsevier Science Publishing Co., Inc.
- 415. St-Germain, G and Summerbell, R. (1996). Champignons filamenteux d'intérêt médical. Caractéristiques et idenfication. -314 p. Belmont, Star Publishing Company.
- 550. Pieckova, E. and Wilkins, K. (2004). Airway toxicity of house dust and its fungal composition. Ann Agric.Environ Med. 11[1], 67-73.
- 581. Pharmacia Diagnostics AB. (2007). Allergy & autoimmunity. Diagnostics product catalogue 2007. internet , 1-48. Pharmacia.
- 594. Claeson, A. S., Levin, J. O., Blomquist, G., and Sunesson, A. L. (2002). Volatile metabolites from microorganisms grown on humid building materials and synthetic media. J Environ Monit. 4[5], 667-672.
- 603. Nielsen, K. F., Gravesen, S., Nielsen, P. A., Andersen, B., Thrane, U., and Frisvad, J. C. (1999). Production of mycotoxins on artificially and naturally infested building materials. Mycopathologia. 145[1], 43-56.
- 605. Gravesen, S., Nielsen, P. A., Iversen, R., and Nielsen, K. F. (1999). Microfungal contamination of damp buildings--examples of risk constructions and risk materials. Environ Health Perspect. 107 Suppl 3:505-8., 505-508.
- 635. Charpin-Kadouch, C., Maurel, G., Felipo, R., Queralt, J., Ramadour, M., Dumon, H., Garans, M., Botta, A., and Charpin, D. (2006). Mycotoxin identification in moldy dwellings. J Appl.Toxicol. 26[6], 475-479.
- 724. Samson, RA, Hoekstra, ES, and et al. (1984). Introduction to food and airbone fungi. 6th, -389 p. Baarn, Centralalbureau voor Schimmellcultures, Institute of the Royal Netherlands Academy of Arts and Sciences.
- 726. Jiao, R. H., Xu, S., Liu, J. Y., Ge, H. M., Ding, H., Xu, C., Zhu, H. L., and Tan, R. X. (2006). Chaetominine, a cytotoxic alkaloid produced by endophytic Chaetomium sp. IFB-E015. Org Lett. 8[25], 5709-5712.
- 727. Ding, G., Song, Y. C., Chen, J. R., Xu, C., Ge, H. M., Wang, X. T., and Tan, R. X. (2006). Chaetoglobosin U, a cytochalasan alkaloid from endophytic Chaetomium globosum IFB-E019. J Nat.Prod. 69[2], 302-304.
- 728. Yu, J., Yang, S., Zhao, Y., and Li, R. (2006). A case of subcutaneous phaeohyphomycosis caused by Chaetomium globosum and the sequences analysis of C. globosum. Med Mycol. 44[6], 541-545.
- 729. Hattori, N., Adachi, M., Kaneko, T., Shimozuma, M., Ichinohe, M., and Iozumi, K. (2000). Case report. Onychomycosis due to Chaetomium globosum successfully treated with itraconazole. Mycoses. 43[1-2], 89-92.
- 732. Wilson, S. C., Wu, C., Andriychuk, L. A., Martin, J. M., Brasel, T. L., Jumper, C. A., and Straus, D. C. (2005). Effect of chlorine dioxide gas on fungi and mycotoxins associated with sick building syndrome. Appl.Environ Microbiol. 71[9], 5399-5403.
- 737. Barron, M. A., Sutton, D. A., Veve, R., Guarro, J., Rinaldi, M., Thompson, E., Cagnoni, P. J., Moultney, K., and Madinger, N. E. (2003). Invasive mycotic infections caused by Chaetomium perlucidum, a new agent of cerebral phaeohyphomycosis. J Clin Microbiol. 41[11], 5302-5307.
- 740. Yeghen, T., Fenelon, L., Campbell, C. K., Warnock, D. W., Hoffbrand, A. V., Prentice, H. G., and Kibbler, C. C. (1996). Chaetomium pneumonia in patient with acute myeloid leukaemia. J Clin Pathol. 49[2], 184-186.
- 741. Abbott, S. P., Sigler, L., McAleer, R., McGough, D. A., Rinaldi, M. G., and Mizell, G. (1995). Fatal cerebral mycoses caused by the ascomycete Chaetomium strumarium. J Clin Microbiol. 33[10], 2692-2698.
- 746. Sekita, S., Yoshihira, K., Natori, S., Udagawa, S., Sakabe, F., Kurata, H., and Umeda, M. (1982). Chaetoglobosins, cytotoxic 10-(indol-3-yl)-[13]cytochalasans from Chaetomium spp. I. Production, isolation and some cytological effects of chaetoglobosins A-J. Chem.Pharm.Bull.(Tokyo). 30[5], 1609-1617.
- 767. Pieckova, E. (2003). In vitro toxicity of indoor Chaetomium Kunze ex Fr. Ann Agric.Environ Med. 10[1], 9-14.
- 797. Udagawa, S., Muroi, T., Kurata, H., Sekita, S., Yoshihira, K., Natori, S., and Umeda, M. (1979). The production of chaetoglobosins, sterigmatocystin, O-methylsterigmatocystin, and chaetocin by Chaetomium spp. and related fungi. Can J Microbiol. 25[2], 170-177.
- 800. Sekita, S., Yoshihira, K., Natori, S., Udagawa, S., Muroi, T., Sugiyama, Y., Kurata, H., and Umeda, M. (1981). Mycotoxin production by Chaetomium spp. and related fungi. Can J Microbiol. 27[8], 766-772.
- 807. Lee, T. G. (2003). Health symptoms caused by molds in a courthouse. Arch Environ Health. 58[7], 442-446.
- 876. Andersen, B. and Nissen, A. T. (2000). Evaluation of media for detection of Strachybotrys and Chaetomium species associated with water-damaged buildings. International Biodeterioration & Biodegradation 46, 111-116.
- 902. Purdy, C. W., Layton, R. C., Straus, D. C., and Ayers, J. R. (2005). Virulence of fungal spores determined by tracheal inoculation of goats following inhalation of aerosolized sterile feedyard dust. Am J Vet.Res. 66[4], 615-622.
- 989. Centre de recherche sur la conservation des documents graphiques. (2007). Moisissures et biens culturels. Ministère de la culture et de la Communication, France .
- 1153. Fogle, M. R., Brasel, T. L., Wilson, S. C., and Straus, D. C. (2007). 'Mycotoxin identification in moldy dwellings'. J Appl.Toxicol. 27[2], 198.
- 1175. Khan, N. N. and Wilson, B. L. (2003). An environmental assessment of mold concentrations and potential mycotoxin exposures in the greater Southeast Texas area. J Environ Sci.Health A Tox.Hazard.Subst Environ Eng. 38[12], 2759-2772.
- 1395. Reboux, G. (2006). Mycotoxins: health effects and relationship to other organic compounds. Revue Française d'Allergologie et d'Immunologie Clinique 46[3], 208-212.
- 1527. Vesper, S., McKinstry, C., Ashley, P., Haugland, R., Yeatts, K., Bradham, K., and Svendsen, E. (2007). Quantitative PCR analysis of molds in the dust from homes of asthmatic children in North Carolina. J Environ Monit. 9[8], 826-830.
- 1528. Vesper, S., McKinstry, C., Haugland, R., Wymer, L., Bradham, K., Ashley, P., Cox, D., Dewalt, G., and Friedman, W. (2007). Development of an Environmental Relative Moldiness Index for US Homes. J Occup Environ Med. 49[8], 829-833.
- 1734. Guppy, K. H., Thomas, C., Thomas, K., and Anderson, D. (1998). Cerebral fungal infections in the immunocompromised host: a literature review and a new pathogen--Chaetomium atrobrunneum: case report. Neurosurgery. 43[6], 1463-1469.
- 1735. Al-Aidaroos, A., Bin-Hussain, I., El, Solh H., Kofide, A., Thawadi, S., Belgaumi, A., and Al, Ahmari A. (2007). Invasive chaetomium infection in two immunocompromised pediatric patients. Pediatr Infect Dis J. 26[5], 456-458.
- 1736. Aspiroz, C., Gene, J., Rezusta, A., Charlez, L., and Summerbell, R. C. (2007). First Spanish case of onychomycosis caused by Chaetomium globosum. Med Mycol. 45[3], 279-282.
- 1739. Bashyal, B. P., Wijeratne, E. M., Faeth, S. H., and Gunatilaka, A. A. (2005). Globosumones A-C, cytotoxic orsellinic acid esters from the Sonoran desert endophytic fungus Chaetomium globosum. J Nat.Prod. 68[5], 724-728.
- 1741. Kobayashi, M., Kanasaki, R., Sato, I., Abe, F., Nitta, K., Ezaki, M., Sakamoto, K., Hashimoto, M., Fujie, A., Hino, M., and Hori, Y. (2005). FR207944, an antifungal antibiotic from Chaetomium sp. no. 217 I. Taxonomy, fermentation, and biological properties. Biosci.Biotechnol.Biochem. 69[3], 515-521.
- 1743. Paterson, P. J., Seaton, S., Yeghen, T., McHugh, T. D., McLaughlin, J., Hoffbrand, A. V., and Kibbler, C. C. (2005). Molecular confirmation of invasive infection caused by Chaetomium globosum. J Clin Pathol. 58[3], 334.
- 1744. Jiao, W., Feng, Y., Blunt, J. W., Cole, A. L., and Munro, M. H. (2004). Chaetoglobosins Q, R, and T, three further new metabolites from Chaetomium globosum. J Nat.Prod. 67[10], 1722-1725.
- 1745. Fujimoto, H., Sumino, M., Okuyama, E., and Ishibashi, M. (2004). Immunomodulatory constituents from an Ascomycete, Chaetomium seminudum. J Nat.Prod. 67[1], 98-102.
- 1747. Tomsikova, A. (2002). Causative agents of nosocomial mycoses. Folia Microbiol (Praha). 47[2], 105-112.
- 1749. Segal, R. and Kusne, S. (1999). Cerebral fungal infections in the immunocompromised host: a literature review and a new pathogen--Chaetomium atrobrunneum: case report. Neurosurgery. 45[1], 200.
- 1750. Thomas, C., Mileusnic, D., Carey, R. B., Kampert, M., and Anderson, D. (1999). Fatal Chaetomium cerebritis in a bone marrow transplant patient. Hum Pathol. 30[7], 874-879.
- 1751. Lesire, V., Hazouard, E., Dequin, P. F., Delain, M., Therizol-Ferly, M., and Legras, A. (1999). Possible role of Chaetomium globosum in infection after autologous bone marrow transplantation. Intensive Care Med. 25[1], 124-125.
- 1753. Schulze, H., Aptroot, A., Grote-Metke, A., and Balleisen, L. (1997). [Aspergillus fumigatus and Chaetomium homopilatum in a leukemic patient. Pathogenic significance of Chaetomium species]. Mycoses. 40 Suppl 1:104-9., 104-109.
- 1754. Aru, A., Munk-Nielsen, L., and Federspiel, B. H. (1997). The soil fungus Chaetomium in the human paranasal sinuses. Eur Arch Otorhinolaryngol. 254[7], 350-352.
- 1755. Guarro, J., Soler, L., and Rinaldi, M. G. (1995). Pathogenicity and antifungal susceptibility of Chaetomium species. Eur J Clin Microbiol Infect Dis. 14[7], 613-618.
- 1759. Sue, M. A., Gordon, E. H., and Freund, L. H. (1992). Utility of additional skin testing in "nonallergic" asthma. Ann Allergy. 68[5], 395-397.
- 1760. Stiller, M. J., Rosenthal, S., Summerbell, R. C., Pollack, J., and Chan, A. (1992). Onychomycosis of the toenails caused by Chaetomium globosum. J Am Acad Dermatol. 26[5 Pt 1], 775-776.
- 1765. Woods, G. L., Davis, J. C., and Vaughan, W. P. (1988). Failure of the sterile air-flow component of a protected environment detected by demonstration of Chaetomium species colonization of four consecutive immunosuppressed occupants. Infect Control Hosp Epidemiol. 9[10], 451-456.
- 1766. Costa, A. R., Porto, E., Lacaz, Cda S., de Melo, N. T., Calux, Mde J., and Valente, N. Y. (1988). Cutaneous and ungual phaeohyphomycosis caused by species of Chaetomium Kunze (1817) ex Fresenius, 1829. J Med Vet.Mycol. 26[5], 261-268.
- 1767. Ito, Y. and Ohtsubo, K. (1987). Teratogenicity of oral chaetochromin, a polyphenolic mycotoxin produced by Chaetomium spp., to mice embryo. Bull Environ Contam Toxicol. 39[2], 299-303.
- 1769. Manning, R. O. and Wyatt, R. D. (1984). Comparative toxicity of Chaetomium contaminated corn and various chemical forms of oosporein in broiler chicks. Poult.Sci. 63[2], 251-259.
- 1770. Hoppin, E. C., McCoy, E. L., and Rinaldi, M. G. (1983). Opportunistic mycotic infection caused by Chaetomium in a patient with acute leukemia. Cancer. 52[3], 555-556.
- 1771. Gupta, J., Pathak, B., Sethi, N., and Vora, V. C. (1981). Histopathology of Mycotoxicosis produced in Swiss albino mice by metabolites of some fungal isolates. Appl Environ Microbiol. 41[3], 752-757.
- 1772. Stark, A. A., Kobbe, B., Matsuo, D., Buchi, G., Wogan, G. N., and Demain, A. L. (1978). Mollicellins: mutagenic and antibacterial mycotoxins. Appl Environ Microbiol. 36[3], 412-420.
- 1775. Christensen, C. M., Nelson, G. H., Mirocha, C. J., Bates, F., and Dorworth, C. E. (1966). Toxicity to rats of corn invaded by Chaetomium globosum. Appl Microbiol. 14[5], 774-777.
- 1829. Undagawa, S.-I., Toyazaki, N., and Yaguchi, T. (1997). A new species of Chaetomium from house dust. Mycoscience 38[399], 402.
- 1872. Von Arx, J. A., Guarro, J., and Figueras, M. J. (1986). Ascomycete Genus Chaetomium. Nova Hedwigia Beihfte [84].
- 2123. Walsh, T. J. and Groll, A. H. (1999). Emerging fungal pathogens: evolving challenges to immunocompromised patients for the twenty-first century. Transpl.Infect Dis. 1[4], 247-261.
- 2207. de Hoog, G. and Guarro, J. (1995). Atlas of clinical fungi. Baarn, Centraalbureau voor Schimmelcultures.
- 2255. Beezhold, D. H., Green, B. J., Blachere, F. M., Schmechel, D., Weissman, D. N., Velickoff, D., Hogan, M. B., and Wilson, N. W. (2008). Prevalence of allergic sensitization to indoor fungi in West Virginia. Allergy Asthma Proc. 29[1], 29-34.
- 2342. Burge, H. A. (1985). Fungus allergens. Clin Rev Allergy. 3[3], 319-329.
- 2497. Jesenska, Z., Pieckova, E., and Bernat, D. (1993). Heat resistance of fungi from soil. Int J Food Microbiol. 19[3], 187-192.
- 2522. Vesonder, R. F., Lambert, R., Wicklow, D. T., and Biehl, M. L. (1988). Eurotium spp. and echinulin in feed refused by swine. Appl Environ Microbiol. 54[3], 830-831.
- 3095. Foundation for Allergy Research in Europe. (1984). Atlas of moulds in Europe causing respiratory allergy. Knud Wilken-Jensen et Suzanne Gravesen. -110. Danemark, ASK Publising.
- 3284. Hollister-Stier Laboratories. (2009). Allergenic extracts : Molds. Hollister-Stier Laboratories .
- 3285. Federal Drug Administration (FDA). (2008). Biological products deviation reporting (BPDR). Non-blood product codes. 3-29-2009.
- 3289. Fogle, M. R., Douglas, D. R., Jumper, C. A., and Straus, D. C. (2007). Growth and mycotoxin production by Chaetomium globosum. Mycopathologia. 164[1], 49-56.
- 3313. Kung'u, J. (2006). Presence of Chaetomium in an indoor environment: what are the implications? Mould & Bacteria Reviews [4].
- 3314. al-Nahdi, M., al-Frayh, R., and Hasnain, S. M. (1989). An aerobiological survey of allergens in al Khobar, Saudi Arabia. Allerg.Immunol.(Paris.). 21[7], 278-282.
- 3317. Liebeskind, A. (1972). Mycological problems in occupational allergies. J Asthma.Res. 10[1], 71-73.
- 3318. UniProt Consortium. (2009). Taxonomy : fungi metazoa group. Site de UniProt . 4-6-2009.
- 3337. Guarro, J. and Gene, J. (1995). Opportunistic fusarial infections in humans. Eur.J Clin.Microbiol.Infect.Dis. 14[9], 741-754.
- 3358. Gu, J. D., Mitton, D. B., Ford, T. E., and Mitchell, R. (1998). Microbial degradation of polymeric coatings measured by electrochemical impedance spectroscopy. Biodegradation. 9[1], 39-45.
- 3360. Patel, A. M., Ryu, J. H., and Reed, C. E. (2001). Hypersensitivity pneumonitis: current concepts and future questions. J Allergy.Clin.Immunol. 108[5], 661-670.
- 3361. Griffin, J. F., Rampal, A. L., and Jung, C. Y. (1982). Inhibition of glucose transport in human erythrocytes by cytochalasins: A model based on diffraction studies. Proc.Natl.Acad.Sci.U.S.A. 79[12], 3759-3763.
- 3362. Mohovic, J., Gambale, W., and Croce, J. (1988). Cutaneous positivity in patients with respiratory allergies to 42 allergenic extracts of airborne fungi isolated in Sao Paulo, Brazil. Allergol.Immunopathol.(Madr.). 16[6], 397-402.
- 3363. Millner, P. D. (1977). Radial growth responses to temperature by 58 Chaetomium species, and some taxonomic relationships. Mycologia 69, 492-502.
- 3364. Steinman, H. (2006). m208 Chaetomium globosum. Site de ImmunoCAP - InVitroSight . ImmunoCAP - InVitroSight. 4-21-2009.